Shoulder arthroscopy is a minimally invasive type of shoulder surgery. Surgeons operate through small incisions with the aid of a small camera that they insert into your shoulder joint (arthroscope). If you need surgery on your shoulder, arthroscopy can make for an easier recovery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
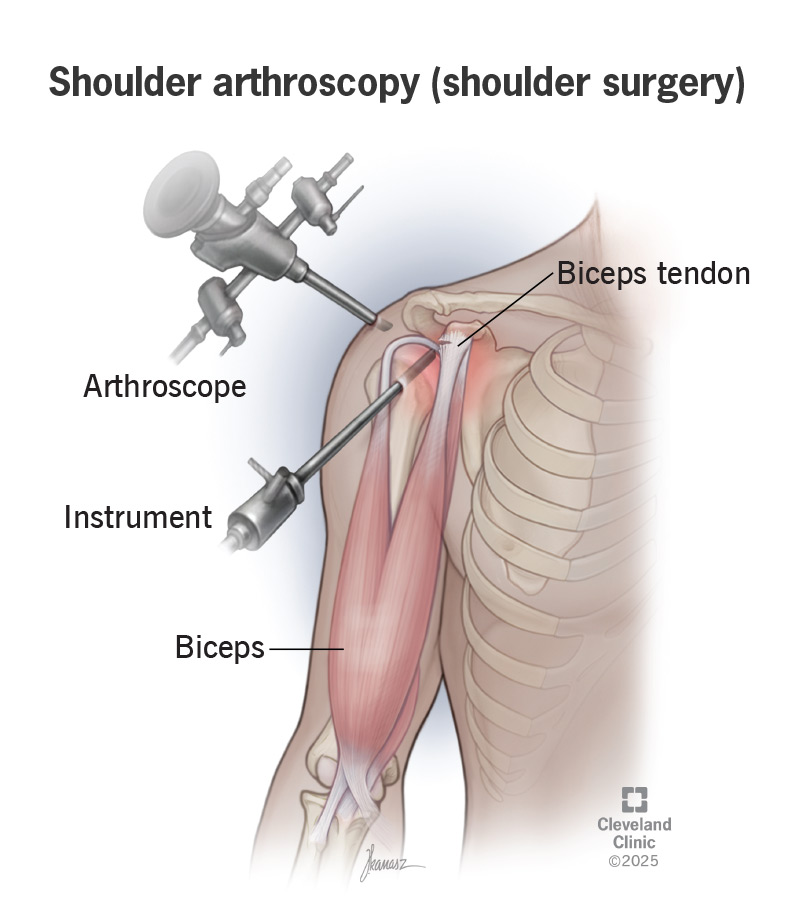
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/shoulder-arthroscopy)
Shoulder arthroscopy is minimally invasive surgery on your shoulder joint. Surgeons use arthroscopy to access your joints with tiny cameras and tools through small incisions. It allows them to diagnose and treat many joint conditions while causing you minimal pain and recovery time. If you have unexplained shoulder pain or an injury that needs repair, your provider might suggest arthroscopic shoulder surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Shoulder arthroscopy is an option to treat almost any shoulder condition, unless it’s an emergency or a whole shoulder replacement surgery. For example, you might have arthroscopic shoulder surgery to treat:
Surgery isn’t the first treatment for most shoulder conditions. But it may be the next option when other treatments don’t work. If you do need shoulder surgery, arthroscopy can make the experience easier.
Arthroscopic shoulder surgery is usually an outpatient procedure. Unless you have special health risks, you’ll probably go home shortly afterward. Most procedures take between one and two hours.
A healthcare provider will discuss your anesthesia options in advance. You’ll likely have a regional nerve block to numb your shoulder and arm. You may also have sedation or general anesthesia with it.
Here’s what happens during shoulder arthroscopy:
Advertisement
You may spend an hour or two in the recovery room after your operation. Your healthcare team will monitor your recovery and discuss home care. They’ll set your arm in a sling before you go home.
Arthroscopic shoulder surgery is generally very safe. But with any procedure, there’s a small risk of:
Arthroscopy makes the recovery from surgery a little easier because you won’t have a large wound to heal. The smaller incisions heal faster and tend to cause less pain and fewer complications in the process. This also allows you to start your physical rehabilitation sooner. Starting to move your shoulder sooner means it won’t be as stiff in the beginning, and there’s less risk of contracture.
After your operation, a healthcare provider will explain how to take care of yourself at home, including:
After your wounds have healed, a physical therapist will show you how to start gradually exercising your shoulder to regain flexibility and strength. Physical therapy will be an essential part of your recovery.
Recovery from shoulder surgery has several stages. The first stage is when your incisions are healing. With arthroscopy, this stage takes one to two weeks. But recovering the full use of your shoulder can take much longer. After the first phase of recovery, you’ll begin your physical rehabilitation. A physical therapist will guide this stage of your recovery, which may take three to six months or longer.
While arthroscopy makes recovery quicker overall, there’s still a wide range of recovery times between different types of shoulder procedures. A minor procedure heals more quickly than a more extensive one. Your overall health and how well you keep up with your physical rehabilitation will also make a difference. Your healthcare provider can tell you more about what to expect in terms of recovery time.
During your recovery, healthcare providers advise that you:
Advertisement
Call your provider right away if you develop:
If you’ve struggled with persistent shoulder pain that other treatments haven’t fixed, it might be time to consider shoulder surgery. Arthroscopy offers a minimally invasive way for surgeons to diagnose and treat many shoulder conditions. While the recovery can take some patience and persistence, there’s hope of real relief at the end. Your healthcare team will walk you through each step of the process.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s orthopaedic providers can help relieve constant shoulder pain with the latest surgery options and personalized recovery plans.
