Hypertrophic cardiomyopathy (HCM) is a complex type of heart disease that makes your heart muscle too thick. It can disrupt blood flow and cause symptoms that come and go, like shortness of breath and dizziness. Medications and procedures are available to relieve symptoms and prevent complications like sudden cardiac arrest.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
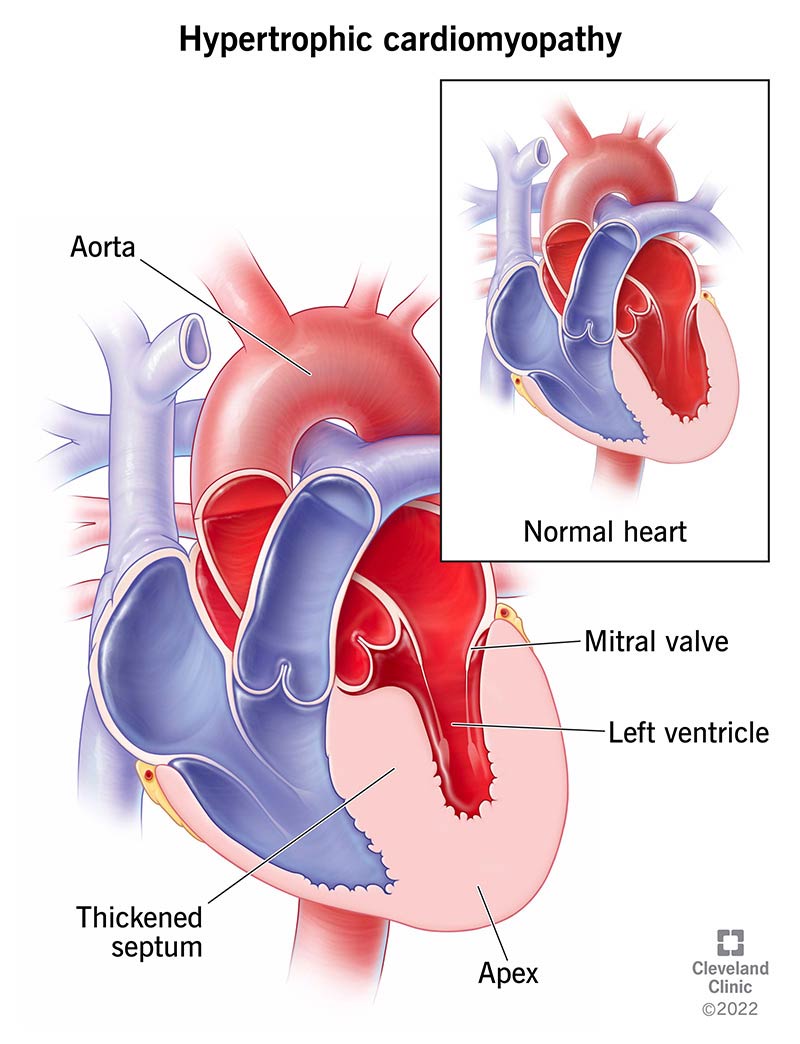
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/17116-hypertrophic-cardiomyopathy)
Hypertrophic cardiomyopathy (HCM) is a genetic form of heart disease that thickens areas of your heart muscle. It most often affects the wall dividing your lower heart chambers. A thicker wall means there’s less open space inside your heart’s main pumping chamber (left ventricle). This may limit how much blood your left ventricle holds and sends to your body. HCM affects anywhere from 1 in 200 to 1 in 500 people around the world. Many people are undiagnosed.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
HCM is a lifelong condition that can get worse over time. In some people, it never leads to symptoms or issues. Others have symptoms that disrupt their life. The most severe cases can cause your heart to suddenly and unexpectedly stop beating. Hypertrophic cardiomyopathy is the most common cause of sudden cardiac death in athletes under age 35.
That may sound scary. But there’s good news. With medications or procedures to treat HCM, you can often live as long as those who don’t have HCM. And you can feel better from day to day. The key is learning if you’re at risk — for example, if HCM runs in your family. Getting a diagnosis early lets a healthcare provider monitor and treat the condition over time.
There are two main types:
The obstructive form is more common. It generally causes more severe or disruptive symptoms earlier in life.
Advertisement
HCM symptoms tend to come and go based on what you’re doing at the time. You’re more likely to have symptoms if you’re dehydrated, stressed, drinking alcohol, eating heavy meals or exerting yourself.
Common HCM symptoms include:
If you have any of these symptoms, it’s crucial to see a healthcare provider.
Some people have no symptoms and only find out they have HCM when certain signs show up on imaging tests. These include:
Most cases of HCM are genetic and run in families. That means you inherit certain gene changes that can cause the condition to develop. HCM follows an autosomal dominant inheritance pattern. So, if you have an HCM gene, there’s a 50% chance that your biological child will inherit it.
The severity of HCM can vary widely, even within the same family. Just because you inherit the gene doesn’t mean you’ll develop the disease. Some people are carriers. This means they have the altered gene but never develop symptoms or complications. Others start to have symptoms at some point in life — often during the teen years or young adulthood.
Healthcare providers can find a gene change in some people who have HCM. It often affects the MYBPC3 or MYH7 genes, but there are also other responsible genes, including ones that scientists haven’t found yet.
Most people with HCM don’t experience complications, especially if they receive treatment. But it’s possible for HCM to cause serious or life-threatening issues, including:
Healthcare providers diagnose hypertrophic cardiomyopathy based on a medical history, physical exam and testing. Your provider will review your health records and ask about your symptoms. They’ll also want to know if anyone in your family has a history of HCM, other heart diseases or sudden death. They’ll listen to your heart and lungs with a stethoscope. If you have HCM, they may hear a heart murmur.
Advertisement
Tests you may need include:
HCM screenings are routine tests for people at risk due to family history. It’s important to get screenings if you have a biological parent, sibling or child with the condition.
If you learn about a family member’s diagnosis, tell your healthcare provider. They’ll explain the screening schedule you should follow. Typically, this involves having an echo test and an EKG every few years.
Advertisement
If you have an HCM diagnosis, tell your family. They’ll need to talk to their healthcare providers about getting screened. Healthcare providers are especially concerned with first-degree relatives, including biological parents, siblings and children.
Together, you and your heart doctor (cardiologist) will decide on a treatment plan based on how HCM is affecting you and your risk for serious issues, like ventricular arrhythmias and cardiac arrest, both of which can be fatal. The goal of treatment is to reduce symptoms and lower the risk of complications. Your treatment plan may include monitoring, medications and/or procedures.
This means you go in for routine check-ups and tests, like echo tests and EKGs. Monitoring might be all you need for many years. That’s often the case if your risk for complications is low and you don’t have symptoms.
If you’re receiving treatments, like medications, your doctor will also keep a close eye on your condition. You’ll have tests every so often to check your heart function and assess your risk level. These tests allow your doctor to adjust your treatments as needed.
The medications your doctor prescribes for you depend on the type of HCM you have. The U.S. Food and Drug Administration (FDA) recently approved medications called cardiac myosin inhibitors to treat obstructive HCM. These medications, which target the root cause of the disease, include:
Advertisement
Researchers haven’t found targeted treatments for nonobstructive HCM yet. Although there are clinical trials looking at possible medications, the main treatments that your doctor may prescribe to help your heart work better and reduce symptoms include:
For either form of HCM, you may need medications to manage heart disease risk factors or abnormal heart rhythms.
You may need surgery or a less invasive procedure to manage symptoms or lower your risk of cardiac arrest. Options include:
You’ll need to see your cardiologist regularly so they can check on your heart. They’ll let you know how often to come in for follow-up visits based on the condition’s severity and your treatment plan.
If possible, it’s best to receive care through a hospital system that’s experienced in treating hypertrophic cardiomyopathy.
HCM is a lifelong condition. Your outlook depends on how severely the condition affects blood flow and whether you develop symptoms or complications. Some people inherit HCM but stay free of symptoms their whole lives. Others develop issues at a young age. Seeing your cardiologist regularly and following your treatment plan can help protect your heart and overall health.
Your cardiologist will guide you on things like:
In the past, hypertrophic cardiomyopathy often shortened a person’s life expectancy. But advances in treatment have changed that. Today, with treatment, HCM usually doesn’t affect how long a person lives. Your cardiologist can give you the most accurate sense of what to expect in your case.
Getting a heart disease diagnosis like hypertrophic cardiomyopathy can be overwhelming. Try to take a deep breath. There are ways to manage the condition and protect your health. Your cardiologist will guide you through a management plan that’s tailored to your needs. Lean on loved ones for help, too, especially when it comes to changes you’re making in your daily life.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic offers personalized diagnosis and the latest treatments for hypertrophic cardiomyopathy.
