
On the golf course, in the locker room or at the clubhouse, Cleveland Municipal Court Judge Michael Nelson, Sr. and his friends will discuss just about anything.
Judge Nelson, a longtime attorney and community activist, was surprisingly taken aback after he shared the news of his recent treatment for prostate cancer with 10 of his buddies. As he soon discovered, all 10 of them had also undergone or were about to face treatment for issues with their prostate, a small gland that is part of the male reproductive system.
“Every one of the guys had a prostate-related experience, and not one of us had talked to each other about it? I was stunned,” recalls Judge Nelson, 75, who was elected as a judge in 2017. “I would have liked to have known about what they had gone through when I was diagnosed, but I had no idea any of them had experienced it. I said, ‘We’ve got to do something about this!’”

While golfing with his friends, Judge Nelson shared his prostate cancer journey. He was surprised to learn most of his male friends had faced similar medical issues and never spoke about them. (Courtesy: Judge Michael Nelson)
Following his successful treatment for prostate cancer in February 2023, Judge Nelson has been advocating to all men – especially Black men, who are at high risk of prostate cancer – that they get their prostate checked as part of regular health screenings.
“Men aren’t going to talk about this unless someone brings up the subject first,” he continues. “Too often, men ignore health symptoms. Those of us who have been through a procedure need to be candid about it. We need to encourage other guys to get checked. Because if you have prostate cancer, you’re not going to be able to ignore it away.”
Numerous studies reveal many men may often fail to get regular checkups or screenings for prostate cancer, which occurs in about one in nine American men, killing about 33,000 annually. The rate is even higher among Black men. According to the National Cancer Institute, the incidence of prostate cancer among Black men is 64% higher than Caucasian men.
A simple and effective method for prostate screening is a common blood test that measures a man’s prostate-specific antigen (PSA) levels. If the level is found to be elevated, other tests, such as an MRI and/or biopsy of the prostate, can determine whether treatment is needed.
Judge Nelson receiving care at Hillcrest Hospital. (Courtesy: Judge Michael Nelson)
Because so many men may not regularly get their health screenings, Cleveland Clinic conducts its annual MENtion It campaign to raise awareness of prostate cancer and other health issues that are specific to men.
According to Zeyad Schwen, MD , a urologist at Cleveland Clinic Hillcrest Hospital who led Judge Nelson’s treatment, early detection through preventive measures are essential to diagnosing prostate cancer and other treatable conditions while they are still in curable stages.
“It’s important men, especially those at high risk for prostate cancer, get their PSA level checked annually or every two years,” says Dr. Schwen. Men and people who were assigned male at birth should have their first PSA screening test and exam between ages 45 and 50. Those who have a family history of prostate cancer, should consider having their first prostate screening evaluation between ages 40 and 45.
“If a problem is found early, it can be monitored, or if needed, treated. We support what Judge Nelson is doing to get the word out, as a lot of people respect him in the community,” says Dr. Schwen.

Judge Nelson continues his advocacy work in the community by spreading awareness around the importance of getting regular check-ups and prostate cancer screenings. (Courtesy: Judge Michael Nelson)
While Judge Nelson has regularly gotten PSA blood tests for more than a decade, it was during a pre-operative physical examination before he was to undergo hip replacement surgery urologist Samuel Haywood, MD, discovered his PSA level had elevated.
A prostate MRI soon after revealed the presence of two abnormal lesions on the right side of his prostate. A subsequent biopsy, performed by Dr. Schwen revealed the presence of cancer.
Judge Nelson and Dr. Haywood reviewed a number of treatment options. Because Judge Nelson’s cancer was determined to be at an intermediate risk level, he would likely be eligible for a relatively noninvasive method of focal ablation therapy, which pinpoints treatment to the specific areas of the prostate where the cancer is located.
Drs. Haywood and Schwen, with input from Judge Nelson, determined the best course of therapy would be high-intensity focused ultrasound (HIFU). As Dr. Schwen explains, HIFU is an outpatient procedure, conducted under general anesthesia, that involves the use of a small HIFU probe that is inserted into the rectum.
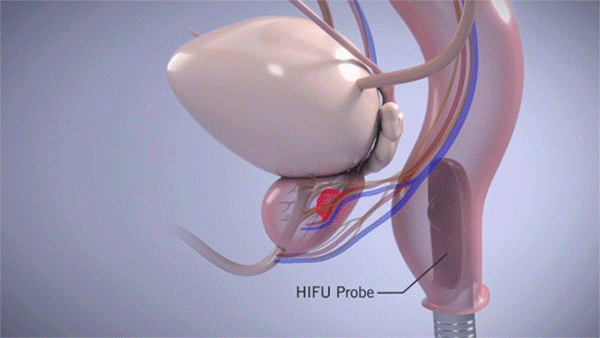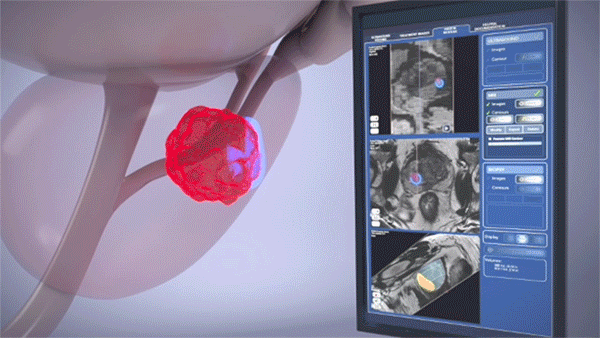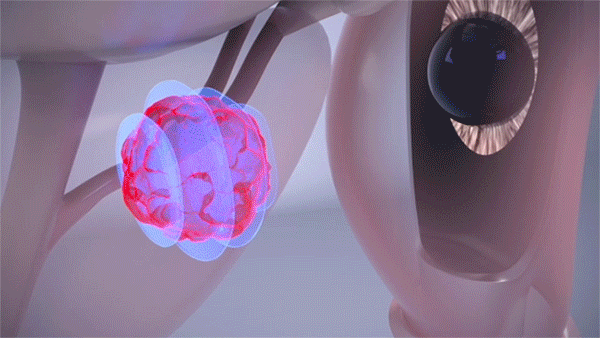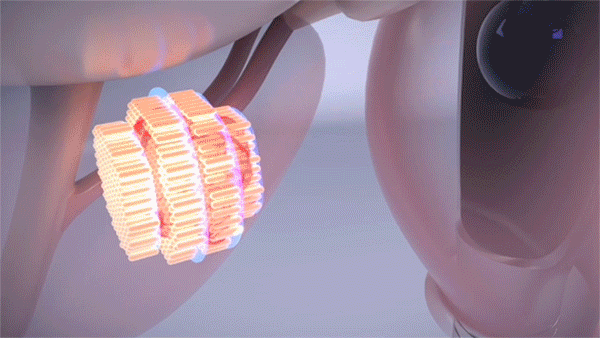
High-intensity focused ultrasound or HIFU is a noninvasive procedure that uses the energy of sound waves to pinpoint, heat and kill prostate cancer cells. (Courtesy: Cleveland Clinic)
Once in position, the device emits very high-intensity and highly focused sound waves that destroy (or ablate) the targeted tissue area without harming surrounding tissue. While the possibility of swelling in the area required Judge Nelson to be fitted with a catheter for a couple of days, he praised the guidance and support he received from nurse practitioner Laura Pita, CNP, who eased his nerves and calmly guided him through every step of the postoperative process.
He recovered quickly and was back to work and the golf course in just a matter of weeks. Follow-up exams have detected no remaining presence of cancer, and Judge Nelson is eager to share his experience with other men.

Judge Nelson with his wife, Donna. (Courtesy: Judge Michael Nelson)
“I hope Judge Nelson’s courage and the example he sets will inspire other men to talk with their doctor about their health and ask about prostate cancer screening,” adds Dr. Haywood.
Judge Nelson states any qualms or fears men may have about prostate-related issues are nothing to worry about compared to the possible outcomes of ignoring symptoms or failing to get screenings and treatment.
Related Institutes: Cleveland Clinic Cancer Center, Glickman Urological & Kidney Institute

