You have a dislocated jaw when your lower jawbone (mandible) pulls away from your temporomandibular joints (TMJ). A dislocated jaw is a medical emergency because you may not be able to eat or speak. Healthcare providers treat a dislocated jaw by gently pushing your lower jaw back where it belongs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
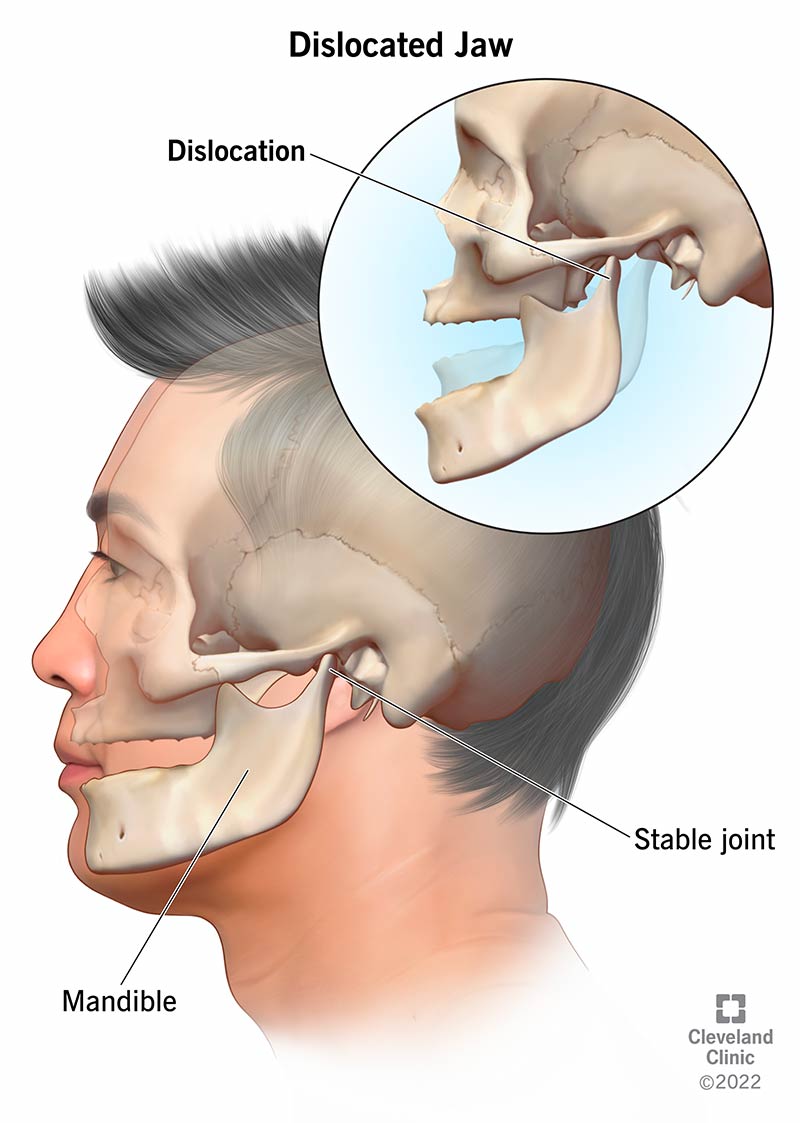
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/24882-dislocated-jaw)
You have a dislocated jaw when your jaw joint or temporomandibular joint (TMJ) is out of place. Your TMJ includes the joints, jaw muscles and ligaments that connect your lower jaw to your skull. These parts work together so you can open and close your mouth.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
When you dislocate your jaw, the parts that help your jaw move can’t work as they should. A dislocated jaw is a medical emergency because you may not be able to eat or speak. Healthcare providers treat a dislocated jaw by gently pushing your lower jaw back where it belongs.
A dislocated jaw is very painful. If you’ve dislocated your jaw, you also may notice:
You could dislocate your jaw while doing everyday activities such as yawning widely, laughing or biting into an oversized sandwich. You also may dislocate your jaw if someone or something hits your jaw.
You may be more likely to get a dislocated jaw if you:
Providers will ask how your jaw was dislocated, such as whether it happened from an injury or because you had your mouth wide open while eating or laughing or during a dental or medical procedure. They’ll examine your lower jaw. They may do an X-ray to determine the gap between your skull base and your temporomandibular joint.
Advertisement
Interestingly, medical historians credit Hippocrates for the way providers treat dislocated jaws today. Hippocrates was a Greek physician, known as the “father of medicine,” who lived from about 460 B.C.E. He called the treatment “molchlicon.” Now, it’s called manual reduction.
In manual reduction, a provider gently moves your jawbone back into place. They place their thumbs on either side of your mouth and their fingers under your chin, and then, they gently push your jawbone back where it belongs. (You’ll receive a sedative, local or general anesthesia, for this procedure.)
A dislocated jaw is a medical emergency. Providers can treat your dislocated jaw with manual reduction if they’re able to treat it right away. Delaying treatment makes manual reduction less likely to work.
If your jaw continues to pull away from your TMJ, your healthcare provider may recommend surgery. The surgery tightens the connection between your jawbone and your temporomandibular joint by shortening the ligaments that connect your jawbone to your skull or providing a free pathway for self-reduction.
It takes most people about six weeks to recover from manual reduction for a dislocated jaw. Your provider may recommend the following steps to help you to recover:
Not always. Some people dislocate their jaws because they were hit in the jaw. You may not be able to avoid all the situations where that can happen, such as vehicle accidents or falling on your face. That said, there are things you can do:
Giving yourself time to heal is the best way to take care of yourself. People who have manual reduction typically recover within six weeks. But it may be a few months before your jaw heals completely.
Advertisement
Unfortunately, dislocating your jaw once increases the risk you’ll dislocate it again. Go to the emergency room if you dislocate your jaw again.
You have a dislocated jaw when your jaw joint or temporomandibular joint (TMJ) is out of place. You can dislocate your jaw by laughing with your mouth wide open, by biting into an oversized sandwich or if something or someone hits your jaw hard. No matter how it happens, a dislocated jaw is a medical emergency. The quicker you seek treatment, the more likely you’ll be able to heal without needing surgery.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Temporomandibular joint (TMJ) disorders cause more than jaw pain. Cleveland Clinic’s TMJ specialists offer the latest treatments for relief.
