With cervical ectropion, the glandular cells on the inner portion of your cervix become visible from the outside. It’s a harmless variation, or difference, in the way your cervix appears. It rarely causes symptoms and isn’t cause for concern.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cervical ectropion means that the cells typically inside your cervix are visible on the outside of it. It isn’t a concerning condition. It’s just a difference in the way that cervical cells appear.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The outer and inner parts of your cervix consist of two types of cells:
Cervical ectropion happens when glandular cells are visible on the outside of your cervix. Your gynecologist may notice it during a routine pelvic exam or Pap smear. It’s most common if you’re of reproductive age. Anywhere from 17% to 50% of females have this variation.
Since it’s a harmless condition, your healthcare provider likely won’t mention you have it.
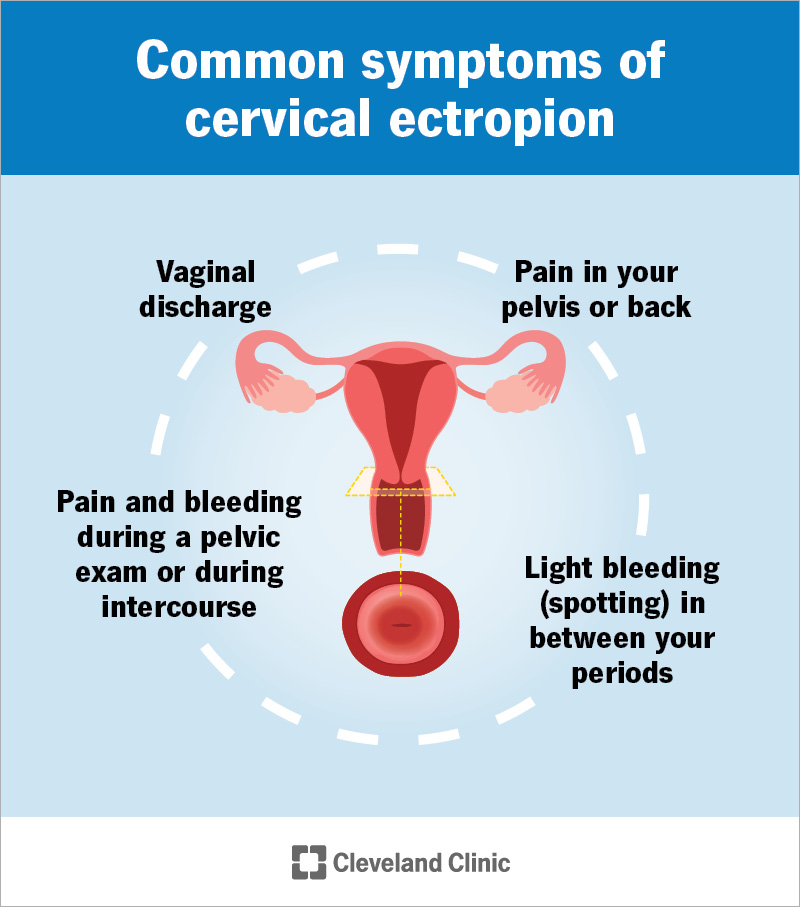
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23053-cervical-ectropion)
Cervical ectropion doesn’t usually cause symptoms. But in rare cases, it can cause symptoms like:
If you have these symptoms, it’s more likely that something other than cervical ectropion is causing them. See your healthcare provider if you notice changes so you can get a correct diagnosis.
Advertisement
Increased estrogen levels can cause cervical ectropion. Because of this, you’re more likely to have cervical ectropion during:
Taking estrogen-progestin contraceptives and cervical tears during childbirth may also lead to cervical ectropion. If you’ve gone through menopause, you’ll rarely have it.
There’s no need to diagnose cervical ectropion. Many women don’t even know they have it. Rather, it’s something your healthcare provider may notice during a test or procedure for something else, like a pelvic exam or colposcopy.
Cervical ectropion rarely needs treatment. It tends to go away on its own over time. But if you have symptoms that affect your quality of life, treatment can help. Your healthcare provider will want to make sure your symptoms are coming from cervical ectropion and not something else.
They may prescribe boric acid suppositories to lessen symptoms. More intensive procedures can destroy cells that may be causing symptoms, including:
Healthcare providers used to call cervical ectropion “cervical erosion.” But this name is misleading. Cells don’t wear away (erode) with cervical ectropion. Instead, your cervix turns inside out. This makes the glandular cells covering its inner portion visible from the outside.
Cervical ectropion isn’t cancer and doesn’t increase your risk of cancer. But cervical cancer and cervical ectropion can cause the same symptoms, like bleeding after sex. This is why it’s important to see your healthcare provider if you’re having symptoms.
Yes. Cervical ectropion isn’t a cause of infertility. It has no negative effects on pregnancy or the fetus.
The term may sound overly medical, but don’t be concerned if you learn you have cervical ectropion. It’s just a way healthcare providers describe a difference in how your cervix appears. In the rare case you have symptoms from it, your healthcare provider can offer treatment options. Look to them for guidance.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
