A bicornuate uterus is shaped like a heart, appearing to have an indent at the top. A typical uterus is rounded at the top. It’s a condition you’re born with. Surgery can fix it.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
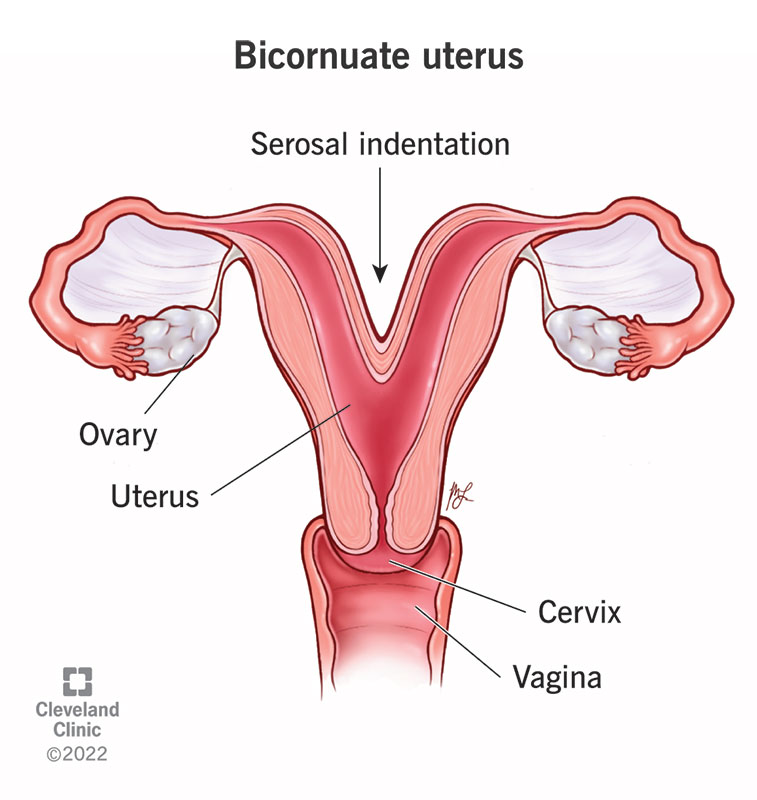
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22798-bicornuate-uterus)
A bicornuate uterus means your uterus is shaped like a heart. A typical uterus is shaped like an upside-down pear. The wide, round part of the pear resembles the top portion of the uterus. If your uterus is bicornuate, the top of your uterus dips down at the middle, making it look like a heart.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A typical uterus is one hollow cavity. It’s made to expand during pregnancy. If you have a bicornuate uterus, the top of your uterus is separated by a piece of tissue. This can cause problems during pregnancy because your uterus may not expand.
A bicornuate uterus is a condition you’re born with. Most people won’t know they have one until they have several miscarriages or a pregnancy complication. If you become pregnant with a bicornuate uterus, there’s an increased risk of preterm labor and other pregnancy complications.
About 0.4% of girls are born with a bicornuate uterus.
Symptoms could include:
In some cases, you may not realize you have a heart-shaped uterus because you don’t have symptoms. Or you could have symptoms, but they may seem normal to you because you don’t know any differently.
You’re born with a bicornuate uterus. The uterus develops in a fetus around week 12 of pregnancy. During development, the Müllerian ducts normally fuse to form one uterine cavity. With a bicornuate uterus, the ducts don’t merge. Experts aren’t completely sure why this happens.
You have a higher risk of endometriosis if your uterus is irregularly shaped. But there aren’t any serious complications of a bicornuate uterus outside of pregnancy. You won’t be able to use an intrauterine device for birth control due to the shape of the cavity.
Advertisement
If you’re pregnant and have a bicornuate uterus, you’re at a higher risk for:
Most people aren’t aware they have a bicornuate uterus until they have several miscarriages. Your healthcare provider may discover the condition while they’re looking for the cause of the miscarriages or preterm labor.
Sometimes, your provider may find a heart-shaped uterus during a routine prenatal ultrasound or because of painful periods.
After a pelvic exam, they’ll use several imaging tests to diagnose a bicornuate uterus:
Your provider may describe your bicornuate uterus as either partial or complete. These terms refer to how far your uterus dips down at the top:
Surgeons can treat a bicornuate uterus with a procedure called metroplasty. During the procedure, they reshape your uterus by removing the tissue that causes the heart-shaped appearance. But surgery usually isn’t necessary. It’s typically only for people with repeat miscarriages or a history of pregnancy complications.
Many people with the condition have no symptoms and can have a healthy pregnancy without surgery. Your pregnancy care provider may just monitor you more during your pregnancy. You’ll likely have more prenatal ultrasounds. This is so your provider can see the size and shape of your uterus, the fetus and the placenta.
If your provider recommends surgery, they’ll explain the procedure, its risks and your chances of having a successful pregnancy afterward.
Contact a healthcare provider if you experience pelvic pain during your period or during sex. These could be signs of an underlying condition.
If you’re pregnant with a bicornuate uterus, you should contact your healthcare provider immediately if there are any signs of labor, like contractions or your water breaking.
Some questions to ask your healthcare provider about this condition are:
Advertisement
Yes, you can get pregnant. Fertility usually isn’t affected. But the shape of your uterus puts you at a slightly higher risk for pregnancy complications. Your healthcare provider will discuss any precautions you should take during pregnancy.
Maybe. Your uterus may not expand as much as a typical uterus. This could lead to preterm labor or the fetus being in a breech position. Your pregnancy care provider may recommend a C-section delivery if this is the case. You’re also at a higher risk of postpartum hemorrhage.
No, they’re different. Uterus didelphys is when you’re born with two uteruses (double uterus).
If you have a bicornuate uterus, it’s completely natural to have questions or concerns. Talk openly with your healthcare provider about how this diagnosis affects your life and your plans for children. They can help you understand any potential risks and support you every step of the way. Know that many people with this condition don’t need surgery and go on to have healthy pregnancies.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
