You might have a ventral hernia if you see or feel a bulge pop out occasionally through your front abdominal wall. Hernias are common and usually aren’t an urgent concern, but most will eventually need surgical repair.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
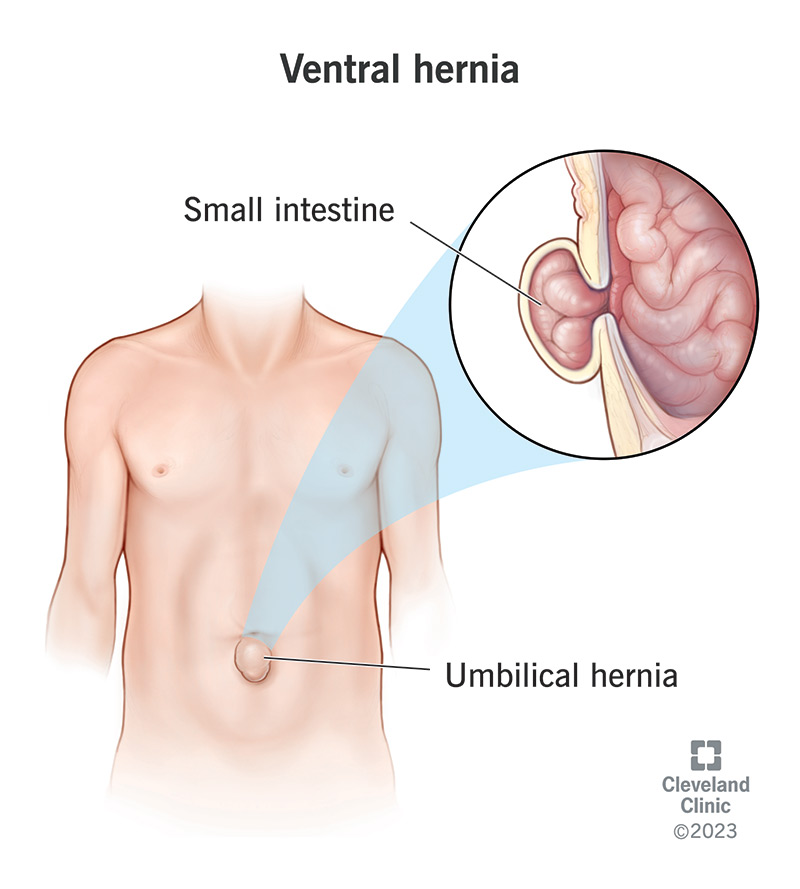
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/16531-ventral-hernia)
A ventral hernia is a hernia that occurs through your front abdominal muscles. “Ventral” refers to your front or belly area. A hernia is when one of your internal organs or tissues bulges through an opening in the wall of its body cavity. Most (but not all) hernias come through one of your abdominal walls.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Different types of ventral hernias occur in different locations in your front abdominal wall. They include:
The first sign of a ventral hernia is usually a visible bulge that appears somewhere in your front abdominal wall. You may only see it emerge occasionally during certain activities or in certain positions that contract your abdominal muscles. For example, you might see your ventral hernia when you’re:
Some people, but not all, can also feel their hernia. You might feel it when it pops out, or when some movement pulls it, compresses it or pinches it. It might feel like a tug, a dull ache or a sharper pain. Hernia pain is a sign of a larger hernia that may be at risk of getting stuck (incarcerated) while it’s out.
Advertisement
Other symptoms of a more complicated hernia might include:
A hernia pushes through a weakness in the muscle or tissue barrier that contains it. Sometimes, the weakness is already there at birth. Other times, a single event, like an injury or surgery, causes it. And sometimes, it happens over time through gradual wear and tear. Often, it’s more than one of these.
Common contributing causes of ventral hernias include:
Most hernias can move in and out of their opening, appearing and disappearing. But moving in and out continues to weaken the tissues around it. Over time, the opening gets bigger, and so can the hernia, meaning more of your organ or tissue bulges through. This is when complications can happen.
The bigger a hernia becomes, the more at risk it is of getting stuck or “incarcerated” in the opening. This pinches or compresses the hernia, causing pain and potentially obstructing the organ. You could end up with a blocked intestine, or its blood supply could be cut off (strangulation). This can cause tissue death.
A healthcare provider will usually find a ventral hernia during a physical exam. If they don’t see it right away, they’ll have you try different positions or actions to make it emerge. In some cases, they might take images to see the hernia more clearly. This might mean an abdominal ultrasound, CT scan or MRI.
If they can see and feel the hernia physically, they’ll examine it up close and check to see if they can gently push it back in. This tells them how serious it is and how soon it might need treatment. They’ll also ask you detailed questions about your symptoms, health history and possible causes, such as:
Most ventral hernias should be repaired eventually, but not necessarily right away. A hernia that doesn’t cause you any symptoms and that you can still push back in probably isn’t a serious risk. But hernias do tend to worsen over time, and as they do, they can become more dangerous and more difficult to fix. A ventral hernia that can’t be pushed back in is a potential emergency and should be evaluated in the ER.
Advertisement
Healthcare providers recommend ventral hernia repair when:
If your child is born with an umbilical hernia, it will usually heal by itself in a few years. If it doesn’t, their provider will recommend umbilical hernia surgery at that time to prevent it from growing bigger.
The goal of ventral hernia surgery is to repair the hole in your abdominal wall so the hernia can’t come through it again. Surgery restores the shape and tone of your abdominal wall by closing the hole and bringing the muscles back into position. Surgeons may use surgical mesh to reinforce the wall.
Ventral hernia surgery is common and usually simple. General surgeons perform around 350,000 ventral hernia repair operations in the U.S. each year. They can often use minimally invasive methods, which means smaller incisions and a shorter recovery time. But some people need open abdominal surgery.
Your surgeon will decide the best method to use to approach your hernia. The options are:
Advertisement
Not all ventral hernias need to be repaired with mesh, especially if they’re small epigastric or umbilical hernias. But most incisional hernias do because they come through tissue that’s already been cut. Muscle tissue is never quite as strong again after surgery, and hernia repair surgery weakens it again.
Surgeons can choose from several different types of surgical mesh to help repair the hernia:
Surgery is the only way to repair a ventral hernia. But some people can’t have surgery due to other health conditions. If you have a large hernia that can’t be repaired, your healthcare provider may suggest that you wear a special apparatus, like a corset, binder or truss, to hold the hernia in.
Advertisement
Most aren’t serious, but they can become more serious over time. That’s why healthcare providers recommend fixing them before that happens. Elective surgery to prevent serious complications always has better outcomes than emergency surgery to fix serious complications that are already occurring.
Most hernia repairs are simple, and recovery is quick. More complicated hernias might need a more complex operation to fix and a longer recovery. It’s important to take care not to pull or strain the repaired hernia during recovery. An estimated 10% to 20% of ventral hernias may come back after repair.
There are all sorts of reasons why you might develop a ventral hernia. It usually happens gradually, over many years. If you’re aware that something you do every day puts stress on your abdominal muscles, you might be able to turn the tide by changing your habit or treating your chronic condition.
But hernias aren’t always preventable, and if you get one, you’ll be in good company. They’re very common, and so is the surgery to repair them. Your healthcare provider can advise you on when to get your hernia repaired. You may not need to right away, but it’s best to do it before it gets much bigger.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Hernias can be painful – Cleveland Clinic’s experts can help. We are leaders in minimally invasive hernia repair, and abdominal wall reconstruction.
