Iron is one of the minerals in the human body. If you don’t have enough iron, your body can’t make hemoglobin, and you may develop anemia. One way of treating anemia is with intravenous iron, or an iron infusion, which is delivered into a vein through a needle to increase the levels of iron and hemoglobin in your body.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
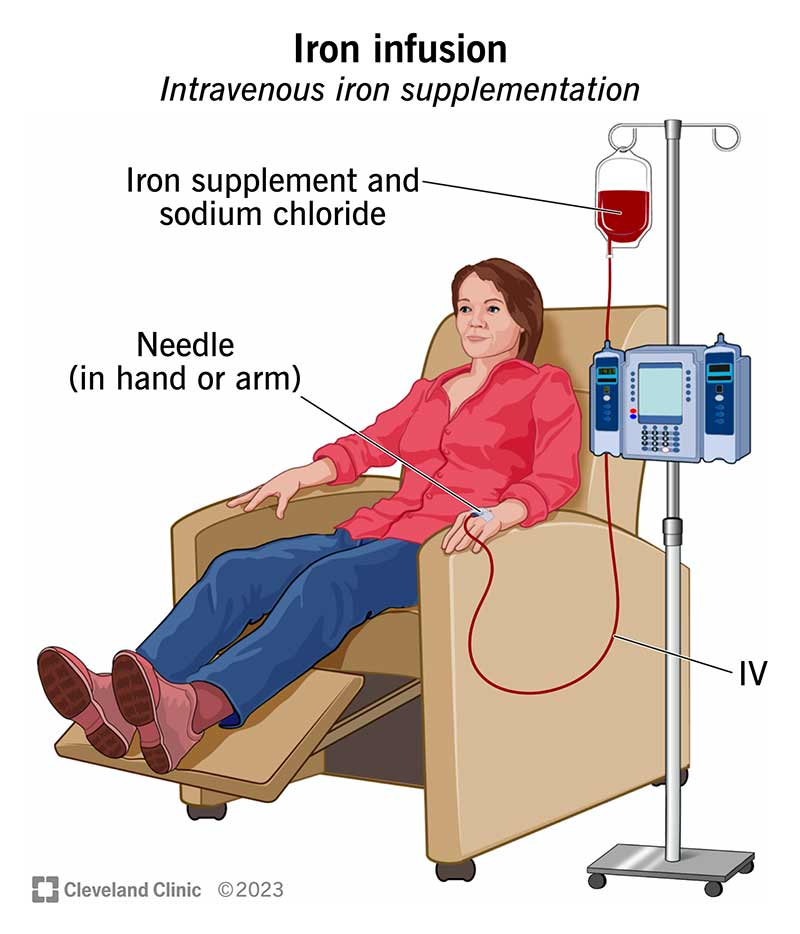
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/14571-iron-infusion-illustration)
An iron infusion is a way to receive iron through a small catheter in your vein. Intravenous (IV) iron supplementation is another name for this. A healthcare provider performs this procedure in a medical office or clinic.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
If you don’t have enough iron, your body can’t make hemoglobin. This protein helps blood carry oxygen throughout your body. With this issue, you may develop anemia. This is known as iron-deficiency anemia, the most common type of anemia.
Factors that can lower your body’s supply of iron include:
Getting iron through an infusion isn’t as common as getting oral (by mouth) iron. Healthcare providers prescribe oral iron supplements first. That works for many people, but some people need to receive iron through an IV if their iron levels are very low.
People usually receive IV iron infusions because they can’t take oral (by mouth) iron. These include people who:
Advertisement
It depends on the reason you’re taking it. Different conditions require different iron levels. A healthcare provider may give you an IV iron infusion sooner for one condition than another.
You may only need one dose of some iron infusions. With others, you’ll need one or two doses over the course of several weeks until your iron level is where it should be. It can take two months to fix your iron level and correct anemia.
A healthcare provider will decide how much iron you need. They can calculate the dose you need based on your weight and how much hemoglobin you have.
Be sure to tell your provider about:
During an iron infusion, a provider will:
An IV iron infusion can take 15 to 30 minutes. You can get a typical dose of 1,000 milligrams of iron in that time.
A healthcare provider will monitor you for 30 minutes or more after your iron infusion. They do this to make sure you don’t have a bad reaction.
It depends on your situation. Normally, it may take several days to a week after you start your iron supplement before you start to feel better. Continue to watch your symptoms and take note of side effects the iron infusion might cause. If you have any questions or concerns, talk to your healthcare provider.
An iron infusion quickly brings your iron level up. Today’s iron infusions work better than the ones in the past. Multiple studies have found that an iron infusion is more effective and more tolerable than the oral (by mouth) kind. They also rarely cause a major reaction.
Iron infusion side effects are usually minimal, but may include:
People usually feel better a few days to a week after an iron infusion.
Advertisement
Contact your provider if you have side effects that you can’t manage.
Taking iron supplements by mouth works for many people, but it may not be right for you. The good news is that iron infusions have come a long way. Today’s medicines can deliver high doses of iron in a short amount of time — usually without a bad reaction. Don’t be afraid to ask questions about your iron infusion if there’s anything that isn’t clear.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
