A robotic cystectomy is a minimally invasive surgery to remove all or part of your bladder. It uses smaller incisions, and it may have a shorter hospital stay and recovery time. Surgeons commonly recommend it to treat bladder cancer. A surgeon may need to create a new way for pee to exit your body. Recovery may take several weeks to months.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
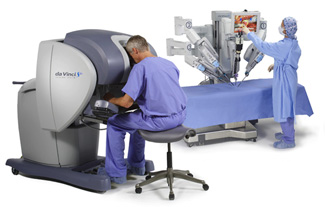
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/da_vinci_1.ashx?h=207&w=325&la=en&hash=68F097596CCDBBD0A9AA903E31B25E1061D69B42)
A robotic radical cystectomy is a type of surgery that removes part of your urinary bladder (robotic partial cystectomy) or your entire bladder (robotic radical cystectomy). It’s different from a traditional cystectomy, in which a surgeon removes part or all of your bladder through a long cut (incision) in your belly area (abdomen). A robotic cystectomy is less invasive — it uses small incisions in your abdomen. A robotic console helps the surgeon guide instruments more precisely in your body. The surgeon then reconstructs your urinary system so pee can move out of your body.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A surgeon may recommend a robotic partial cystectomy if cancer invades only part of your bladder. But most times, a radical cystectomy is necessary to treat bladder cancer. A healthcare provider will explain the type of surgery they recommend for your situation.
Another name for a robotic cystectomy is a robotic-assisted cystectomy (RAC).
A radical cystectomy removes part or all of your bladder.
A surgeon is most likely to perform a robotic cystectomy to treat bladder cancer. But they may recommend a robotic cystectomy to treat conditions that are present at birth that affect your urinary system (congenital urinary anomalies).
A surgeon will remove your bladder and surrounding lymph nodes. In males, the surgeon may also remove reproductive parts, such as:
In females, they may remove reproductive parts, such as:
Robotic cystectomies are becoming more common. One study noted that radical robotic cystectomies increased from 22% of all cystectomies in 2010 to 40% in 2015.
Before a robotic cystectomy, you’ll meet with a healthcare provider. They’ll explain the procedure to you and ask for your consent. They’ll also review your health history and perform a physical exam to make sure you’re healthy enough for surgery.
Advertisement
Tell your provider about any prescription or over-the-counter (OTC) medications you’re taking, including herbal supplements. Aspirin, blood thinners (anticoagulants) and certain herbal supplements can increase your risk of bleeding. Check with a provider before you stop taking any medications.
You should also tell your provider about any allergies you have. These may include:
A provider will give you specific directions on when to stop taking prescription or OTC medications, if necessary. They’ll also give you instructions on when to stop eating and drinking (fast) before the procedure.
A robotic cystectomy team generally includes:
No, a robot doesn’t perform a robotic cystectomy.
The surgical robot enhances the operation by providing three-dimensional, high-definition vision and improved skill (dexterity) in handling the instruments. The urologist uses a surgical console to completely control the robotic arms that hold the instruments. The robotic arms can make precise movements.
During a robotic cystectomy:
When a urologist performs a radical cystectomy, they’ll need to reconstruct your urinary tract in one of three ways so that pee can leave your body. These methods include:
The urologist disconnects a small portion of your small intestine (ileum). They’ll connect the tubes that carry pee from your kidney to your bladder (ureters) to one end of the ileum. The other end of the ileum connects to an opening in your skin (stoma). The stoma is usually close to your belly button on the right side. A plastic appliance (ostomy bag) goes over your stoma to collect pee.
The urologist creates a continent reservoir from parts of your small intestine and large intestine to store pee. They’ll attach the ureters to one end of the reservoir, and the other end of the reservoir connects to a stoma in your abdomen. The reservoir stores pee, and you must empty it periodically with a small drainage tube (catheter) that you insert into the stoma. You don’t need an ostomy bag.
The urologist uses a long piece of small intestine to create a continent reservoir to store pee. The ureters attach to one end of the reservoir, and the other end of the reservoir connects to your urethra. This allows you to pee in a similar way to how you did before surgery. You empty your reservoir periodically by relaxing your pelvic muscles and tensing your abdominal muscles.
Advertisement
A robotic cystectomy takes about six hours to perform.
After a robotic cystectomy, healthcare providers will monitor your overall health, treat your pain and give you recovery instructions. Be sure to follow their instructions, including those regarding physical activity and follow-up appointments.
Once they determine you’re healthy enough, you can go home. Most people go home three to five days after the procedure. You must have someone available to take you home and stay with you for at least a day or two.
The main benefit of a robotic cystectomy is that it treats bladder cancer or other conditions that affect your bladder. Other possible advantages over a traditional open cystectomy include:
Recent studies suggest that robotic cystectomy compares well with traditional open surgery in controlling cancer.
A robotic cystectomy is a major surgery, and any major surgery has risks. Generally, these include:
Advertisement
You may also have changes in how you pee after any bladder surgery. Your bladder is smaller after a robotic partial cystectomy, so you may need to use the bathroom more often. If you have a radical cystectomy, your ability to pee depends on the type of reconstructive surgery you have.
For some males, bladder removal surgery causes sexual side effects. You may have trouble getting and maintaining erections. If providers also remove your seminal vesicles and prostate, you will no longer produce semen.
For females, sexual intercourse is still possible. But it may be uncomfortable if providers remove part of your vagina. A robotic radical cystectomy may also affect the nerves that are responsible for sexual arousal and orgasm.
Your recovery depends on the type of bladder removal surgery you have. Typically, people who undergo a robotic partial cystectomy will have a shorter recovery period than people who undergo a robotic radical cystectomy.
Many people will have a poor appetite and abnormal bowel function (constipation, diarrhea or both) immediately after a robotic radical cystectomy. A complete recovery may take several weeks to months. This is a direct result of using a part of your bowel (intestine) for the urinary diversion.
Advertisement
After robotic cystectomy, contact a healthcare provider immediately if you experience:
Some people with bladder cancer respond well to:
Talk to a healthcare provider about your options.
A robotic cystectomy is a surgical procedure that utilizes a surgical robot to help remove part or all of your bladder. The robot doesn’t perform the cystectomy on its own; a surgeon is in complete control. But the robot allows your surgeon to make exact movements and get a high-definition look inside the surgical area.
It’s normal to have questions about the pros and cons of a robotic cystectomy versus other approaches. You might also wonder how you’ll adjust to changes in your body and daily routine after the procedure. Reach out to a healthcare provider. They’ll answer all your questions, address any concerns, help you adjust and offer the best recommendations for your long-term health.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Hearing you have bladder cancer can leave you worried about what’s next. Cleveland Clinic’s experts are here to guide you forward and craft a treatment plan for you.
