A percutaneous endoscopic gastrostomy (PEG) is a surgery to place a feeding tube. Feeding tubes, or PEG tubes, allow you to receive nutrition through your stomach. You may need a PEG tube if you have difficulty swallowing or can't get all the nutrition you need by mouth.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
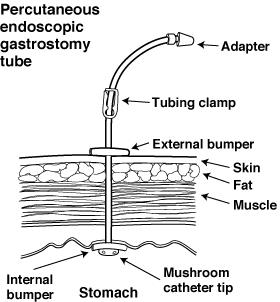
A percutaneous endoscopic gastrostomy (PEG) is a procedure to place a feeding tube. These feeding tubes are often called PEG tubes or G tubes. The tube allows you to receive nutrition directly through your stomach. This type of feeding is also known as enteral feeding or enteral nutrition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You may benefit from a PEG tube if you have difficulty swallowing (dysphagia). Causes of dysphagia may include:
Feeding tubes may also be useful if you have a condition that interferes with how your body processes nutrition. For example, you may benefit from a PEG tube if you have cystic fibrosis or receive dialysis for kidney failure. Someone in a coma may receive a PEG tube to help keep them alive.
Before surgery, you’ll meet with your surgeon to discuss the procedure. You need to tell your provider if you have any heart conditions, bleeding risks or medication allergies.
Depending on your health and underlying conditions, you may need to make medication adjustments. Your healthcare team may recommend changes to:
Don't eat or drink at least eight hours before the surgery. You also need to arrange a ride home after surgery.
Most healthcare providers place PEG tubes with endoscopic surgery. Endoscopic procedures use small incisions and a long, flexible instrument called an endoscope.
Advertisement
On the day of surgery, you receive intravenous (IV) anesthesia and antibiotics. The anesthesia ensures that you remain calm and numb during the procedure. The antibiotic prevents infection.
You may also receive a local anesthetic. A local anesthetic is an injection of numbing medicine. You receive this injection near where your surgeon makes the incision.
During percutaneous endoscopic gastrostomy, your provider:
The entire procedure only takes around 20 to 30 minutes. Usually, you can return home the same day or the next morning.
You’ll feel some pain after a percutaneous endoscopic gastrostomy. This pain might be from the incision. Or you might have cramping from gas buildup in your digestive system. This pain should decrease within 24 to 48 hours.
You’ll have a bandage over the incision site. You may see some drainage around the incision for up to 48 hours. Usually, your surgeon will give you instructions to remove the bandage after one to two days.
After the area around your feeding tube heals, you’ll meet with a dietitian. This specialist explains how to use the PEG tube and starts you on enteral nutrition.
Yes. PEG tubes are about the size of a pen or pencil. You’ll see 6 to 12 inches of the tube coming out of the incision area. Around the tube is a disc called an external bumper. This bumper prevents the tube from going further into your stomach.
At the end of the feeding tube is a small cap or plug. This plug prevents stomach acid or contents from leaking onto your skin or clothes. You can open this plug to receive food, water or medications.
PEG tubes are an important treatment if you have difficulty swallowing or are unable to get adequate nutrition. After G tube placement, you receive specialized nutrition and hydration.
Possible risks of percutaneous endoscopic gastrostomy include:
Your provider will explain the symptoms of a PEG tube complication and when to seek treatment. You’ll need to clean your PEG tube daily to decrease your risk of complications.
Most people with G tubes have no problems or complications after surgery. However, your outlook depends on the underlying medical condition that led to tube placement.
Advertisement
After tube placement, most people receive fluids and liquid nutrition through the tube. People who need PEG tubes because of swallowing problems have restrictions on eating and drinking by mouth. Some people may still eat and drink small amounts through the mouth. Talk with your provider about eating and drinking restrictions.
PEG tubes can last for months or years. They may clog or wear down over time. If your G tube is wearing out, you may notice:
If you need a new PEG tube, your provider can easily replace the tube without invasive surgery or anesthesia. If you don’t need the tube anymore, your provider may remove the tube. The opening in your stomach closes on its own.
If your PEG tube accidentally falls out or moves, contact your healthcare provider right away. The opening in your stomach where the G tube goes can close very quickly. If the tube dislodges, it’s important to receive medical treatment within 24 hours.
A note from Cleveland Clinic
PEG tubes are feeding tubes. They deliver nutrition directly to your stomach. You receive a PEG tube through a short procedure called a percutaneous endoscopic gastrostomy. In this procedure most people can go home the same day. After your feeding tube is placed, you’ll be able to see the tube outside your body. You will need to clean the tube daily and keep it dry between cleanings. If a PEG tube falls out or moves, see a healthcare provider within 24 hours.
Advertisement
Last reviewed on 04/19/2021.
Learn more about the Health Library and our editorial process.