Amblyopia, also known as lazy eye, causes blurry vision in one eye when something affects how your child’s eyes are developing. Their brain starts to ignore the weaker eye. Then, that eye can drift out of position. It’s the most common vision issue that affects kids. It’s very treatable and usually won’t affect your child’s eyes or vision long term.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
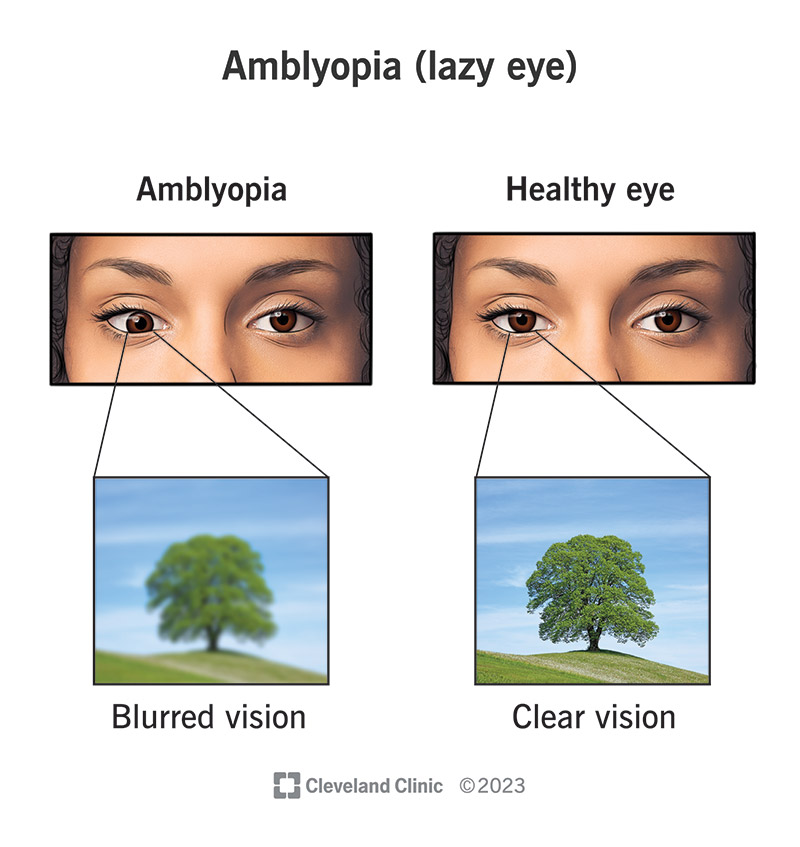
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/10707-amblyopia-lazy-eye)
Amblyopia is an eye condition that affects your child’s ability to see clearly out of both eyes. It usually develops when they’re an infant or very young. It can get worse over time if it’s not treated.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
If your child has amblyopia, one of their eyes has blurry vision, and the other has clear vision. Eventually, their brain will start ignoring the blurry eye. It will only use the eye with clear vision to see. As your child’s brain relies more on the stronger eye, the weaker eye’s vision will get even worse over time. Amblyopia is a serious medical issue. But it responds very well to treatment.
People sometimes refer to amblyopia as lazy eye or lazy vision. Even though these names are common, they’re not accurate. If a child has amblyopia, they’re not lazy, and neither are their eyes. They aren’t choosing to have blurry vision, and it’s not caused by anything they did.
It’s not always easy to tell if your child has amblyopia. Most kids aren’t diagnosed until an eye doctor or their pediatrician gives them an eye exam.
If you do notice symptoms in your child, you’ll probably see changes in how they interact with objects and space around themselves. A child with amblyopia may:
You might not be able to see anything physically different in your child’s eyes. But one of their eyes may look off-center or like it’s drifting in a direction that doesn’t match where your child is looking.
Advertisement
Amblyopia happens when something creates a difference between your child’s eyes and how they focus on objects. The most common causes of amblyopia include:
Any child can develop amblyopia. Some factors make kids more likely to, including:
An eye doctor will diagnose amblyopia. Healthcare providers screen all kids for it during regular check-ups. They’ll perform an eye exam to check your child’s eyes. Your child’s provider will test how well your child can see. They’ll also look for anything that might be affecting how well your child’s eyes work.
Usually, a healthcare provider will diagnose amblyopia before you notice any symptoms at home. Most kids are diagnosed when they’re too young to tell you their vision is worse or changing. Tell your provider or eye doctor if you’ve noticed any changes in how your child holds their head or interacts with objects around them.
Your eye doctor will treat amblyopia by making your child’s brain use their weaker eye to see. This will repair and strengthen the connection between your child’s brain and both their eyes. Eventually, it will correct the amblyopia.
The most common treatments include:
Advertisement
Most kids need amblyopia treatment for at least a few months. Make sure to encourage them to stick with it as long as your eye doctor recommends.
It can be tough for kids to get used to changes in their eyes and vision. That’s especially true when they need amblyopia treatments. Remind your child why it’s important to wear their eye patch and glasses or to use their eye drops. Reward them for sticking with their treatment and encourage them to use their weaker eye as often as they should. And it’s OK if your child feels discouraged sometimes. The important thing is that you’re working together to improve their vision.
Visit a healthcare provider or eye doctor as soon as you notice any changes in your child’s behavior, especially if it seems like they might not be able to see well. Talk to your provider if your child starts favoring one side of their body more than the other, or if they seem less confident when they’re moving around.
Amblyopia is very treatable if it’s diagnosed early. Children who start treatment early in life are much more likely to have improved vision and fewer long-term effects.
Amblyopia can cause permanent vision problems if it’s not treated when your child is young. It’s possible to treat amblyopia in teens, but it takes longer and is usually less effective.
Advertisement
Amblyopia is a common issue that affects kids’ vision. Even though some people refer to it as lazy eye, there’s nothing lazy about it. Remember, amblyopia is a medical condition you can’t prevent, and there’s nothing lazy about your child or their eyes.
The best way to catch amblyopia early is with regular vision tests. Ask your child’s healthcare provider about an eye exam during your child’s check-ups. Your provider or eye doctor will recommend the best ways to correct the amblyopia and help your child have clear vision again.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When a brain injury or another neurological condition affects your eyes, you’ll want the best care. Cleveland Clinic’s neuro-ophthalmology experts can help.
