Allergic rhinitis, also called hay fever, is an allergic reaction that causes sneezing, congestion, itchy nose and watery eyes. Pollen, pet dander, mold and insects can lead to hay fever symptoms. Hay fever can make you feel awful, but you can find relief with lifestyle changes, allergy medications and immunotherapy (allergy shots).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Allergic rhinitis (hay fever) is an allergic reaction to tiny particles in the air called allergens. When you breathe in allergens through your nose or mouth, your body reacts by releasing a natural chemical called histamine. Despite being called hay fever, hay doesn’t cause hay fever and most people don’t get a fever.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Symptoms of hay fever include sneezing, nasal congestion and irritation of your nose, throat, mouth and eyes. Allergic rhinitis isn’t the same as infectious rhinitis, otherwise known as the common cold. Hay fever isn’t contagious. Also, not all rhinitis is allergic. Many people suffer from nonallergic rhinitis resulting in similar symptoms. Inflammation causes rhinitis, not allergens or histamine release.
Several indoor and outdoor allergens cause hay fever. Common hay fever triggers include:
You can have hay fever any time of the year. Seasonal allergies occur in the spring, summer and early fall when trees and weeds bloom and pollen counts are higher. But pollen seasons can vary depending on your location, as well. Perennial allergies can happen year-round. They result from irritants that are always around, such as pet dander, cockroaches and dust mites.
Hay fever is very common. In the United States, around 20% of the population has allergic rhinitis. In 2021, one study found that more than 81 million people had seasonal allergies.
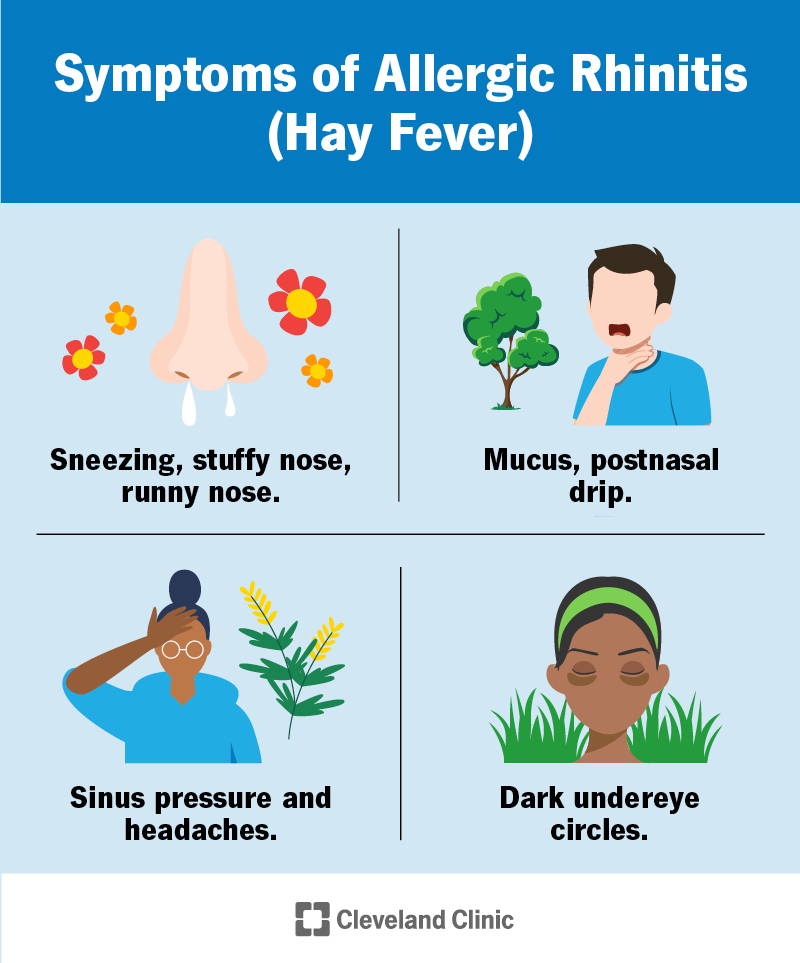
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/8622-allergic-rhinitis-hay-fever)
Hay fever symptoms can appear throughout the year. Outdoor allergies are worse in the spring, summer and early fall depending on where you live. In warm weather, weeds and flowers bloom, and pollen counts are higher. Indoor allergies, such as those from pets and dust mites, can get worse in winter because people spend more time indoors with their windows closed.
Advertisement
Symptoms of hay fever include:
Symptoms of a cold and hay fever are similar, but there are some differences. Itchy, red and watery eyes are common with allergies, but not as common with a cold. A cold is more likely to cause muscle aches and pain or a fever.
Another way people can tell the difference is that allergic rhinitis usually has a trigger, like seasons changing or being around a new pet. Allergies often happen at the same time each year, like in spring and late summer, and they start quickly. On the other hand, a virus causes a cold and you catch viruses from other people. So, you may know it’s a cold if you’ve been around someone with a cold. A cold tends to go away within a week, whereas allergies will stick around until the allergen is out of the air.
Allergic rhinitis occurs when your body’s immune system reacts to an irritant in the air. The irritants (allergens) are so tiny that you can easily inhale them through your nose or mouth.
Allergens are harmless to most people. But if you have hay fever, your immune system thinks the allergen is intruding. Your immune system tries to protect your body by releasing natural chemicals into your bloodstream. The main chemical is called histamine. It causes mucous membranes in your nose, eyes and throat to become inflamed and itchy as they work to eject the allergen from your body.
Allergic rhinitis comes from many allergens, including:
Food allergies can also cause inflammation in your nose and throat. Food allergies can be life-threatening, so get medical help right away if you’re concerned that a certain food is consistently causing allergy symptoms.
Allergies are inherited, which means you’re more likely to have hay fever if you have a parent or immediate family member with allergies. People who have asthma or eczema are also more likely to develop hay fever.
Your healthcare provider will examine you, ask about your symptoms and evaluate you for other conditions, such as a cold or asthma. They can also perform allergy tests.
Advertisement
A blood allergy test measures antibodies to an allergen in a sample of your blood. This blood test is called an immunoglobulin E (IgE) test. It can detect most types of allergies, including food allergies.
Your provider may also recommend a skin prick and/or intradermal test to determine what allergens are causing your symptoms. In a skin prick test, your provider places a small sample of different allergens on your skin (usually on your forearm or back). They scratch or prick your skin with a needle. If you’re allergic to a specific allergen, the area will become red, itchy and irritated in 15 to 30 minutes. Intradermal testing is similar, but your allergist places the allergen underneath your skin. Your skin reacts in the same way it does for a prick test.
Several allergy medications can improve symptoms and help you live with hay fever. These treatments come in many forms, including liquids, pills, eye drops, nasal sprays and injections. Talk to your provider before taking any medication, especially if you’re pregnant or have other health concerns.
Antihistamine medications are available with a prescription or over the counter (OTC). They work by blocking the histamine that your body releases during an allergic response. Antihistamines come as pills, liquids, eye drops, nasal sprays and inhalers. They include:
Advertisement
Antihistamines can cause drowsiness. Avoid alcohol when taking antihistamines, especially if you’re going to drive.
These medications relieve congestion in your nose and sinuses. You can take decongestants by mouth (in pill or liquid form) or use a nasal spray. They include:
Decongestants can increase blood pressure and cause headaches, trouble sleeping and irritability. Nasal decongestants can be addictive when you use them for longer than five days.
These sprays and inhalers reduce inflammation and relieve symptoms of hay fever. The most common nasal sprays are Flonase®, Nasacort® and Rhinocort®. Side effects include headaches, nasal irritation, nosebleeds and cough.
During an allergic reaction, your body releases leukotrienes, histamine and other chemicals that cause inflammation and hay fever symptoms. Available only with a prescription, these pills block leukotriene. The most common leukotriene inhibitor is montelukast (Singulair®). Some people experience changes in mood, vivid dreams, involuntary muscle movements and skin rash when taking this medication.
Advertisement
This treatment works by helping your body learn to tolerate allergens. Your provider gives you a series of injections (allergy shots or subcutaneous immunotherapy) with a small amount of the allergen. Every time you get a shot, your provider increases the amount of the allergen. Over time, your immune system develops immunity to the allergen and stops launching a reaction to it.
In certain circumstances, your provider might recommend immunotherapy in the form of a pill that you place under your tongue called oral immunotherapy. Currently, oral immunotherapy is only available for allergies to trees, grass and dust mites (in the U.S.).
It varies. Most people find relief from hay fever within a few days with medication, but they must take it continuously until the allergen is out of the air. Some people continue to have symptoms of hay fever for several weeks or months, especially if they aren’t taking or can’t take medication to help relieve symptoms.
Hay fever can make you feel miserable, but it generally doesn’t cause serious health problems. Most people with hay fever manage symptoms with lifestyle changes and over-the-counter medication.
People with airborne allergies have a higher risk of ear infections and sinus infections. Because hay fever can make it tough to get a good night’s sleep, you may feel tired during the day. If you have asthma, hay fever can make your asthma symptoms worse.
There’s no way to prevent hay fever, but lifestyle changes can help you live with allergies. You can relieve hay fever symptoms by avoiding irritants as much as possible. To reduce symptoms, you should:
Although hay fever usually doesn’t cause any serious health problems, you should see your provider to rule out other conditions, such as asthma or a sinus infection. Seek care if hay fever symptoms are:
Your provider can help you identify the allergens that are causing a reaction and recommend treatments to help you feel better.
Hay fever is another name for allergic rhinitis. Hay fever mainly refers to seasonal allergic rhinitis, which is the allergies you experience at certain times of the year due to pollen from grass, weeds and trees. But some people use the terms interchangeably.
Seasonal allergies tend to occur in the spring and early fall when pollen from grass, trees and ragweed are more prevalent.
Seasonal allergies tend to happen at the same time each year. They often start suddenly and can last several weeks or until the allergen isn’t in the air anymore. Taking allergy medication to see if it improves your symptoms is one way to know if your symptoms are due to allergies. Checking a weather app or website to see if pollen is high in your area can also help you decide if what you feel is related to seasonal allergies.
Hay fever symptoms can affect your quality of life and keep you from doing the activities you love, but effective treatments are available. Millions of adults and children manage hay fever with medications and lifestyle changes. Talk to your provider about steps you can take to relieve symptoms, breathe easier and feel better.
Learn more about the Health Library and our editorial process.
Cleveland Clinic's health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability, and up-to-date clinical standards.
Cleveland Clinic's health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability, and up-to-date clinical standards.
Allergies can wreak havoc on your life. At Cleveland Clinic, our team of experts can help create a treatment plan that’ll help you breathe easier.
