The pubic symphysis is a joint sandwiched between your left pubic bone and your right pubic bone. It helps your pelvis absorb some of the weight from your upper body before it travels to your lower body. It also helps separate your pelvic bones to prepare for vaginal childbirth.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your pubic symphysis is a joint that connects your left and right pubic bones in your pelvis. Unlike other joints, your pubic symphysis doesn’t move much. Its big job is to hold your pelvic bones in place. It makes small movements that help absorb upper body weight.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You may not think much about this body part until something like pregnancy or a sports injury affects it.
Your pubic symphysis helps with:
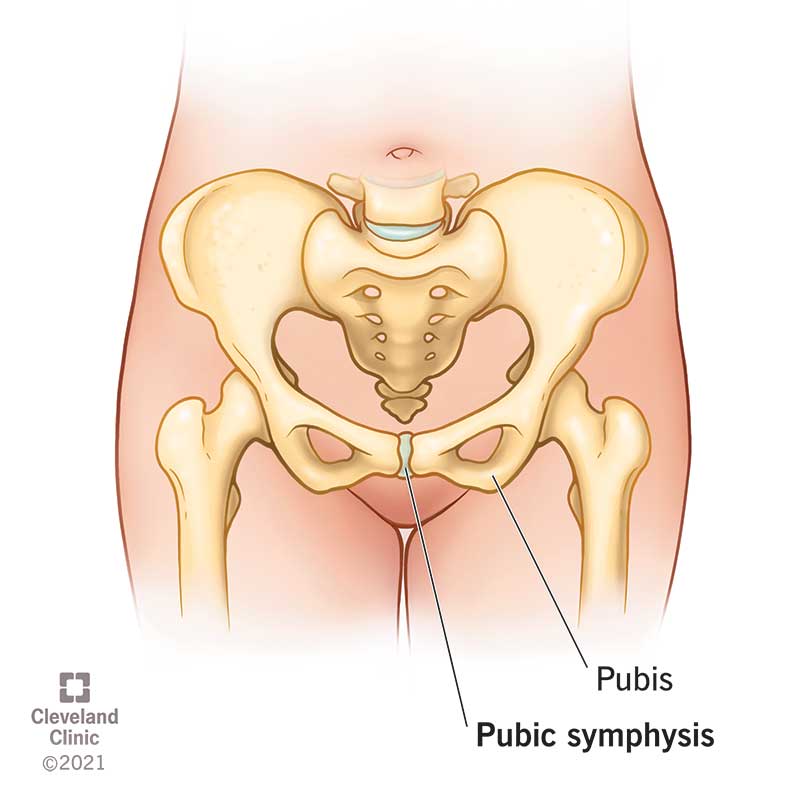
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23025-pubic-symphysis)
Your pubic symphysis is at the bottom of your pelvis, where your left and right pubic bones meet. The joint is wider in the front than it is in the back. It’s in front of your bladder and above your genitals.
Certain tendons connect with ligaments in the pubic symphysis, including:
Your pubic symphysis has two types of cartilage and four ligaments. Together, they make a strong yet flexible connection between your pelvic bones. It allows a little bit of flexibility.
It includes:
Advertisement
Symphysis pubis dysfunction (SPD) is an umbrella term for symptoms you feel because of changes in your pubic symphysis. Two types include:
Pregnancy is a common cause of SPD. During pregnancy, a hormone called relaxin loosens the ligaments that hold your pubic symphysis in place. This can cause issues. Sports injuries are another common cause, especially when you make quick, sharp changes in movement.
Bone and joint conditions that can affect your pubic symphysis include:
Issues with your pubic symphysis often cause pain and an unstable pelvis. You may feel a sharp pain in your pelvis or groin. Sometimes, the pain can spread out across your abdomen, hips and back.
Having trouble with certain movements can cue that something’s wrong. You may feel:
Your healthcare provider can check if a problem with your pubic symphysis is causing your symptoms. They’ll do a physical exam and may recommend imaging tests.
Taking care to strengthen and move your body mindfully is a great way to avoid injury. Your healthcare provider may recommend:
It’s easy to think of the most flexible joints, like your knee and elbow, as the most important ones. But tiny joints like your pubic symphysis have big jobs, too. It helps keep your pelvis in alignment and makes vaginal childbirth possible.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
