Overview
An innovative curriculum
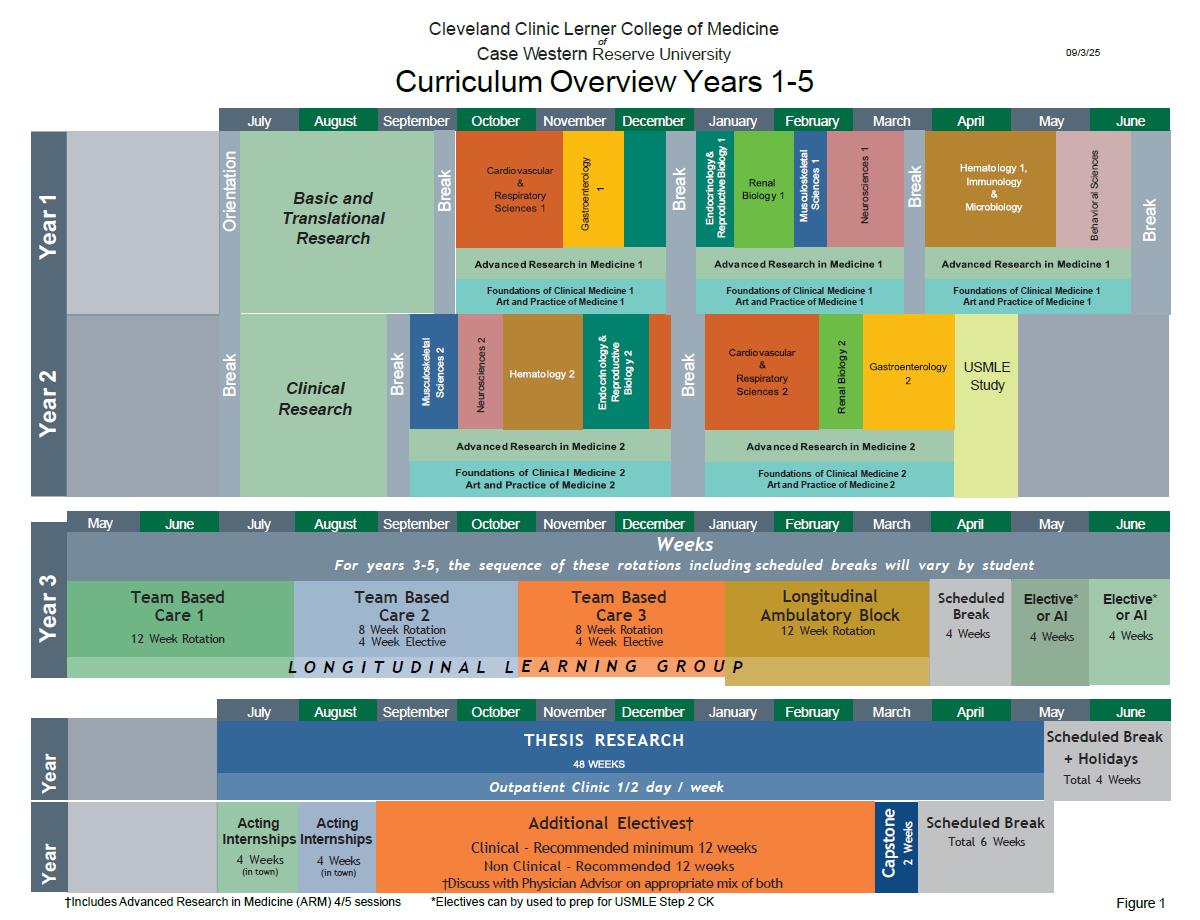
First, view our philosophy video about the curriculum and then take an in-depth look at the five-year curriculum.
- Teaching methods focus on interactive learning and applying knowledge through problem-based learning (PBL), seminars, problem sets, electronic-based curriculum and labs.
- The integrated research curriculum extends throughout the five years and includes hands-on research experience during the first two summers of school and for the 12-month research thesis project.
- The basic science curriculum is organ system-based, with traditional disciplines including anatomy/ histology, pathology, pharmacology, cell biology, physiology, immunology, infectious disease, oncology, bioethics,healthcare systems, bioinformatics and genetics woven through every course. Evidence-based medicine is taught throughout the five years.
- Clinical experiences are integrated throughout the curriculum beginning early in year 1.
- Students are expected to attend and participate in all curriculum activities as part of their professional responsibility.
- A strong commitment has been made to our Humanities in Medicine program, which is an innovative and unique method of teaching students to become skillful and professional physicians.
- During the last three years of the program, CCLCM students take their core clerkship at the Cleveland Clinic and can take clinical electives any of the teaching hospitals in Cleveland affiliated with CWRU. In addition to core clerkship experiences, Cleveland Clinic provides advanced clinical electives, typically taken in year 4, for all CWRU medical students. More than 55 elective rotations in specialty areas are available to CWRU students and other medical students around the country, as available.
- Inter-professional education, or IPE, is all about preparing healthcare students to work together for the benefit of the patient. In today’s healthcare landscape, caring for patients is a team sport. An average hospital patient interacts with dozens of healthcare professionals. Doctors, nurses, therapists, social workers and other professionals work side by side to provide quality, coordinated care. Thus, when students from various healthcare disciplines learn together, they are better able to work together in the future.
Clinical
The clinical curriculum is designed to ensure that all CCLCM graduates develop broad-based clinical expertise. The program uniquely integrates patient care experiences with basic science and research beginning in year 1.
In year 1, students engage in half-day longitudinal case sessions with a primary care physician who meets individually with them every other week. In year 2, the sessions increase to weekly. Students have an opportunity to evaluate new patients and to maintain continuity with past patients during these sessions, and have a close mentoring relationship with faculty.
In year 1, student performance is observed with the goal of providing feedback on the skills being taught in the physical diagnosis and communication skills sessions. Standardized patients participate with faculty and students in their courses.
During the research experience in years 3 through 5, students maintain their relevant clinical experience.
All students:
- Work with a primary care longitudinal preceptor throughout years 1 and 2 to refine physical diagnosis and communication skills, and to longitudinally follow patients
- Maintain patient logs to help track the breadth and depth of clinical exposure, which ensures a comprehensive experience
- Use ongoing assessment of clinical exposure, basic science and clinical competency, and future professional interests to tailor clinical experiences to their needs and interests
These activities are supplemented with communication skills and physical diagnosis sessions using standardized patients, simulation modules and discussion of videotaped sessions with faculty.
Core clinical experience requirements during years 3 through 5 are the same for CCLCM students and students in the University Program. Students from both programs may rotate to any of the major teaching hospitals that are part of the CWRU teaching system.
Research

An Integrated Research Curriculum
The research curriculum begins on the first day and extends through all five years with research topics integrated into the basic science and clinical curricula. Students learn about the interaction between basic and clinical research, how basic science discoveries translate into changes in clinical care and how clinical observations can result in new directions in basic science and research.
Students learn the basic principles of research, including:
- Research design and data analysis.
- Ethical issues such as the use of animals and protection of human subjects in research.
- Critical review of the basic science and clinical research literature.
In addition, students develop and use grant writing and oral presentation skills in school that will help prepare them for the years ahead.
The research curriculum also provides the following:
- Basic Science Research: Every student participates actively in a basic or translational research project in the first summer, preparing a mock research proposal and an oral presentation. The course runs concomitantly with a course in Fundamentals in Molecular Medicine, which introduces models and methodologies used in basic science research.
- Clinical Research: In the second summer, every student participates in a clinical research project while taking courses in applied biostatistics and epidemiology. Also, each student writes a clinical research protocol and presents it at the end of summer.
- Thesis Research: In Year 4, students conduct research on a basic science, translational, clinical, or health systems topic. Thesis research rotation is taken as a contiguous 52-week block that allows up to 4 weeks of vacation. Any variations must be approved by the Research Education Committee. All thesis research rotations are to be done at the Cleveland Clinic, Case Western Reserve University, or an affiliated institution. Only students that have been awarded a NIH, Fulbright, Okinawa Institute of Science and Technology or Sarnoff Fellowship will be permitted to complete their research year outside of Cleveland or Cleveland Clinic Florida Research and Innovation Center. A detailed copy of thesis expectations and guidelines is available in the “Resources” section on the portal or from the Research Education Coordinator.
- Advisors/Preceptors: Each student is assigned a research advisor who helps them navigate the research curriculum as needed. Students work with an assigned basic science researcher (year 1) and select a clinical investigator (year 2) to work with on summer research projects. Students select a research mentor who oversees their thesis project in year 4.
- Opportunities: Research is one of the four cornerstones of Cleveland Clinic and is actively pursued by basic scientists and physicians working in close collaboration. Cleveland Clinic is a world leader in medical breakthroughs and innovations largely because of such collaborations.
Cleveland Clinic offers a broad range of research experiences for CCLCM students. The biomedical research effort here includes:
- Thousands of active, IRB-approved human research protocols.
- Nearly 200 laboratory principal investigators with over $100 million of federal funding support.
- Integrated research curriculum with hands-on research experience.
- Interdisciplinary and disease-oriented research that links basic scientists and clinical investigators in eight disease categories and includes three dozen research programs.
In addition to Cleveland Clinic research opportunities, Cleveland Clinic and Case Western Reserve University and its affiliated teaching hospitals offer a wealth of research experiences at:
- Lerner Research Institute
- Case Western Reserve University research
- Metro Health Medical Center research
- University Hospitals clinical research
- Louis Stokes Cleveland VA Medical Center research
CWRU School of Medicine ranks among the top 25 research institutions in the United States. Research programs are available in a broad range of basic science and clinical disciplines.
Research Seminars: Throughout years 1 and 2, weekly Advanced Research in Medicine (ARM) seminars, integrated with the content of the basic science curriculum, are led by physician investigators and basic science researchers. ARM seminars provide students with exposure to a broad range of research opportunities available to them.
In year 3, ARM sessions focus on developing additional skills needed for research. ARM 4 includes seminars and panel discussions on hot topics in research. ARM 5 provides advice on planning and pursuing a career that includes research.
Journal Club
In the summer of years 1 and 2, students have a journal club aimed at enhancing skills in interpreting and evaluating research literature.
Students are divided into two journal club groups. Each week, one student from the group presents an article while the other students are expected to read the articles carefully and come prepared with questions for the presenters.
Each student is responsible for one paper each summer. The student works with a faculty facilitator to review the paper and presentation before journal club.
Using feedback from faculty and other students on their presentations and on the questions they ask of others, students hone their ability to critically review literature and communicate effectively in this setting.
Combined MD/Master's Degree
If you’re interested in a combined degree to enhance your research skills and expertise, you can coordinate earning a master's degree in selected areas with the MD curriculum.
Most programs require three to nine extra courses, usually concentrated in the first two years, but you can receive some credit toward a master's degree from courses taken as part of the MD program.
We encourage you to develop a thesis project that satisfies the requirements of both the MD and master's degree programs. The remaining master's degree requirements are integrated into the clinical and research program in years 3 through 5. Most master's degree programs are designed to be completed during the five-year program at no extra cost.
If you are in good standing, you can choose from several graduate programs:
- MD in biomedical Investigation with tracks in biochemistry, clinical research scholars, informatics, epidemiology and bio-statistics, nutrition, pathology, pharmacology, biochemistry, physiology and biotechnology.
- MD/MPH.
- MD/MA in bioethics.
- MD/MS in biomedical engineering.
Basic Science
The basic science curriculum is designed to give students a broad-based foundation of knowledge of the complex human biological systems. During the first two years, the basic science curriculum is organized by organ system (e.g., cardio-respiratory, renal biology) with 17 curricular threads basic to medicine (e.g., physiology, anatomy/embryology, cell biology, biostatistics/epidemiology, ethics/humanities) integrated across the courses. Normal cell and organ system function is the focus in year 1; the year 2 curriculum emphasizes abnormal function and reinforces the content from year 1.
Weekly themes guide the organization of each course (e.g., “The Heart as a Pump” during the year 1 cardio-respiratory course) and provide a focus for student learning. When possible, the curriculum integrates the basic science, clinical and research curriculum components around these weekly themes.
A problem-based learning (PBL) case provides the core for each week’s learning objectives. Students are encouraged to apply their knowledge through problem sets and cases during the week’s interactive seminars, which are designed to enrich the understanding of core concepts related to the theme of the week.
Self-directed Learning
The approach to learning basic science is based on adult learning principles where students take responsibility for their own learning and that of their colleagues. PBL and interactive, problem-solving seminars are designed to help students develop extensive skills in learning both independently and in teams — skills that are essential for excellent physicians and successful researchers.
Our competency-based assessment system reinforces these skills by helping students learn to accurately assess their own strengths and weaknesses, and create learning plans for themselves. They also develop teaching skills important to the rest of their career.
Curriculum Structure
During years 1 and 2, each week includes dedicated time scheduled to focus on the basic science curriculum, PBL, labs, seminars, and problem sets.
In Year 1, additional hours are devoted to clinical and research curriculum topics, which are integrated as much as possible with the basic science curriculum.
In Year 2, students have additional hours dedicated to basic science, including an added clinical experience.
Students have most afternoons free to review and prepare educational materials, explore topics in more detail, work toward a master's degree, and engage in extracurricular activities.
Medical Humanities
The study of medical humanities serves to balance the technical and scientific aspects of medicine with its ethical, historical and human dimensions. In recent years, the Association of American Medical Colleges (AAMC) has stressed the importance of including arts and humanities in medical education to prepare students for the challenges of practicing medicine in the 21st century. Since its inception, CCLCM has been committed to this approach by requiring medical humanities coursework and providing ample extracurricular opportunities. In doing so, students complete their medical education with an understanding of the broader context of the meanings of health, illness and healthcare.
Curriculum
Eric Kodish, MD, serves as Director of the Art and Practice of Medicine (APM) courses, which focus on arts and humanities, bioethics, health systems, disability studies and factors that influence health outcomes. The curriculum engages students with theatre, visual arts, poetry, history and film to explore issues of health, illness and healthcare.
Themes of health justice and the role of the physician in society guide the APM curriculum. Throughout their five years at CCLCM, students use reflective writing to pause and contemplate their development as physicians-in-training. Students participate in large- and small-group dialogue, guided by physician preceptors who develop longitudinal mentoring relationships with students.
Hear how students engage with the humanities in this episode of MedEd Thread.
Program in Medical Humanities
Katherine Burke, MFA, leads the Program in Medical Humanities, which offers both curricular and extracurricular opportunities for students to express themselves, engage with our Cleveland neighbors and delve more deeply into the meanings of health and illness. Below are some of the medical humanities initiatives here at CCLCM.
Explore our Humanities program highlights and view student projects.
Learn more about the Program in Medical Humanities in this episode of MedEd Thread.
John P. Murphy Fellowship in Medical Humanities
This two-year fellowship is designed to help MD, PhD or other terminal degree professionals develop expertise in designing, implementing and evaluating educational programs in medical/health humanities and to publish research in the medical/health humanities.
John P. Murphy Medical Humanities Symposium
Focusing on arts and humanities in medical education, this annual symposium will offer an opportunity to showcase the work of CCLCM students and learn from leading scholars in the field who specialize in health professions education.
Stethos Medical Humanities Journal
For over 10 years, Stethos, our journal highlighting humanities and creative works by our students, has provided a platform for creative reflection and a chance to connect through writing, poetry, visual art and photography.
Story Slam
Each year CCLCM students organize Story Slam, an opportunity for Cleveland’s medical students to present original stories, poems, music and more, reflecting on the challenges and joys of being student doctors. Each Story Slam also honors a guest writer who shares their own narrative with students and faculty.
Devising Healthy Communities
Part of the first-year curriculum, this student-led initiative partners students with community organizations to engage in creative collaborations as a way of getting to know and be in right relationship with our Cleveland neighbors. A student leadership team chooses local organizations and coordinates opportunities to come together. Past partner organizations include:
- Edwins Leadership and Restaurant, an organization that offers formerly incarcerated adults a foundation in the culinary and hospitality industries and a support network necessary for long-term success.
- Refresh Collective, a youth empowerment hip-hop and design organization.
- Vel’s Purple Oasis, an urban farm in the neighboring community of Fairfax.
Anatomy & Embryology

The anatomy, embryology and imaging curriculum at the Cleveland Clinic Lerner College of Medicine is distinctive in both its philosophy and design. It provides students with a rigorous, clinically grounded foundation that supports lifelong learning and application in medicine.
Educational Approach
The curriculum is built around case-directed anatomy, in which clinical cases introduce core anatomical concepts and factual knowledge.These concepts are reinforced through hands-on study of prosected fresh cadavers, which are not preserved so that tissue texture, color and spatial relationships remain true to life. Learning is further enhanced through integration with relevant imaging modalities.
Coursework Overview
Anatomy Sessions
Anatomy sessions occur weekly during Year 1 and less frequently during Year 2. Prior to each session, students preview a clinical case accompanied by specific clinical questions and anatomical learning objectives. In class, cases are discussed with clinical faculty, followed by structured time in the cadaver laboratory focused on the anatomical themes of the week.
In the cadaver lab, students rotate through four prosected cadaver stations and review correlated radiographic imaging.The imaging curriculum is extensive in both Years 1 and 2 and is led by radiologists who emphasize clinical relevance and anatomical interpretation.
Basic Science Integration
Anatomy is revisited and reinforced throughout the basic science courses in Year 2, allowing students to integrate structural knowledge with physiology, pathology and other foundational disciplines. Students who wish to gain additional hands-on experience may assist residents in preparing prosections for Year 1 and Year 2 anatomy sessions. Anatomical learning continues during third-year clinical rotations, with advanced surgical anatomy electives available in Years 3 through 5.
Educational Innovation and Technology
To further enhance spatial understanding and individualized learning, anatomy education is supplemented by emerging technologies. Virtual reality platforms allow students to explore anatomy in three dimensions, manipulate structures dynamically and rehearse complex anatomical relationships in an immersive environment. These tools complement cadaveric-based learning by enabling repeated practice and visualization beyond the laboratory, with students able to sign out VR headsets for the academic year to remotely review anatomical concepts, attend virtual anatomy sessions and engage with course content outside of scheduled laboratory time. Through active three-dimensional scanning of cadavers into virtual reality spaces and ongoing innovation in 3D printing, students can revisit complex regions and deepen their understanding beyond the physical laboratory setting.
Education Technology
Technology is used in almost every task that a physician-researcher is required to do such as looking up evidence for treating patients, surveying the scientific and medical literature for research, managing and analyzing data, presenting and disseminating information, communicating with colleagues and patients, and navigating patient medical records.
At CCLCM, we believe that integrating technology appropriately into education, learning, research and patient care throughout the five years of training helps prepare our students for the world of tomorrow. With this in mind, we are committed to providing you with all the appropriate tools and creating the right environment for you to develop a high level of comfort and confidence in using technology for everyday tasks.
Student Web Portal
The Student Web Portal is web-based and accessible without a Secure ID card. The portal’s view can be customized for each student and includes:
Schedule/Calendar: Most learning occurs in small groups, which change several times a year. The system keeps track of your groups, location and learning material. You can download a personalized calendar from the portal to import into your Outlook calendar. You also can access a mobile-friendly version of the portal using any smartphone.
Syllabus: The system provides a customized view of the entire five-year syllabus for each student. Thus, a third-year student can view the cardiopulmonary course she took in the year 1, and the course may appear differently than the cardiopulmonary course a second-year student took in year 1. Students also can find their completed activities by searching in the learning objectives.
Learning Activities: Applications were developed for certain activities such as problem-based learning (PBL). Each PBL case is organized into three parts that are completed over a course of a week. Students in each (PBL) group develop learning objectives and resolve these before proceeding to the next part. The web app allows each group to proceed at its own pace and to upload group-specific learning material to the server.
Resources: A dynamic list of class-specific resources is maintained on the portal. Thus, a first-year student may see a link to basic science research, while a second-year student would see a link to clinical science research.
Contacts: The portal includes information about faculty and fellow students, pager numbers and a web-based alpha-paging application.
Patient Logs in Years 1 and 2
A special feature of the College Program is that you start interacting with patients during your first year of medical school. Patient interactions are done in a safe, controlled environment under the guidance of a longitudinal preceptor. You have access to an online patient-based experience (PBE) system that allows you to:
- Enter your patient logs
- Review learning objectives (clinical skills) for each week or block
- Receive formative feedback based on observed interactions
- Develop your evidence-based medicine skills by formulating clinical questions and searching for and reviewing evidence to answer those questions
- Begin to write "SOAP" notes: subjective, objective, assessment, and plan.
You also will log patients seen through clinical exposure during your research year, approximately one half day per week to maintain your clinical skills.
Curriculum Vitae Builder
A well-formatted, complete and current CV is required when applying for research funding, residency programs and more. Because it can be difficult and time consuming to keep all this information in one place and format it differently for various requirements, we have developed a CV builder that allows you to enter your data and then, when required, produce an appropriately formatted CV with one click.

