Overview

Welcome from the Program Director
Whether you’ve landed on our site because you’re considering applying to our residency, or you’re simply curious to learn more about who we are – Welcome! We hope this website gives you a clear window into what makes our program special.
Our primary focus is to help each resident achieve their goals. We believe there is no ‘one-size-fits-all’ approach to training, which is why our uniquely flexible curriculum – including seven blocks of individually designed ‘tracking’ time – is built-in to give you the space and mentorship required to explore your interests. Whether your passion lies in research, advocacy, education, innovation, global health or clinical excellence, we will be here to support you every step of the way.
As a relatively new program, founded in 2012, we were intentionally structured first and foremost to support resident learning and growth. What sets us apart is a culture built on mutual respect, mentorship and flexibility: a training environment where challenge is paired with support at every level.
We have over 60 faculty members who volunteer their time to residency activities outside of their normal clinical spectrum - our team of faculty and staff are just as collaborative, driven and passionate as the residents we train. Together with our 7 subspecialty Fellowships, we pride ourselves on learning together, supporting each other and growing as a team.
At Cleveland Clinic – consistently ranked among the world’s top hospital systems- our residents train within a high-volume, quaternary care environment. Residents not only manage every day, ‘bread-and-butter’ cases but also participate in the diagnosis and treatment of rare, high acuity, complex referrals. This breadth of exposure, combined with a patient population that spans all backgrounds, ensures a well-rounded, transformative clinical experience. Additionally, the Cleveland Clinic affords incredible resources – from cutting-edge research and innovation teams to leadership development programs and national experts across every subspecialty. If you can dream it, we are committed to helping you achieve it.
Thank you for your interest in our program. We hope you will reach out anytime if you want to get to know us better.
Stacie Jhaveri, MD
Program Director
Lindsey Beffa, MD
Associate Program Director
Erica Newlin, MD
Associate Program Director
Mitch Reider, MD
Associate Program Director
Alexis Scaparotti, MD
Associate Program Director

Melinda MacDonald
Director of Graduate Medical Education Clinical Institutes - Obstetrics & Gynecology, Children's & Primary Care

Erin Hodgson
Residency Program Manager
Tracking Program
Thank you for your interest in Cleveland Clinic's Obstetrics & Gynecology Residency Program. Unlike other residency training programs in the nation, Cleveland Clinic’s ACGME-accredited program affords their residents seven blocks of tracking which means they will have the flexibility, time and support to design their own curriculum.
What is Tracking?
As a new program in 2012, our Cleveland Clinic Ob/Gyn department was not dependent on the presence of residents for clinical practice to occur, therefore was able to build a program from the ground up, dedicated to education over service. To prioritize individual education, 7 blocks of tracking, or individualized elective time, was afforded to allow residents to design their own curriculum targeting areas of interest to them. Initially created as a way to improve surgical skills and operative experiences during residency, this flexible elective time has become a unique opportunity to gain exceptional and focused training in ANY area of interest to YOU.
What if I want to be a Specialist?
Tracking is for everyone, not just those that want to pursue a subspecialty fellowship. Tracking time is flexible, focused and individualized so that you can pursue any area that will support your educational goals
Residents pursuing a specialist career have been able to hone their skills in areas of interest to them with common tracking time spent in menopause, vulvar, and infectious disease clinics, substance abuse clinics as well as outpatient ultrasound and procedural clinics. Many utilize this time to complete AIUM or Robotic training certification if that is something they desire. The options are endless, and our faculty mentors are dedicated to supporting you through any new tracking experience that you want to create.
What if I change my mind and want to pursue a different Subspecialist or go into Specialty practice?
Tracking blocks are simply dedicated time in the curriculum for you to focus your education on areas of interest to you. Unlike other tracking specialties that require you to make a career choice early in your residency training, our tracking blocks are always flexible and always designed by YOU. Tracking time is often utilized to explore different subspecialities, to immerse yourself in a subspecialty of choice or to hone your skills in general Ob/Gyn. Tracking is also ideal for residents that decide to pursue a subspecialty later in their training as they will have built-in tracking time available to work with some of the best mentors in the field who can help support their career journey.
Some examples of innovative tracking experiences:
- Global health trips: residents have utilized tracking to gain experience in global health systems and in Cervical Cancer screening/treatment (ex. India, Rwanda, China and El Salvador)
- Health Literacy and Innovations: residents have dedicated time to collaborate with our Global Health, Communications and Innovations departments to address barriers to patient education and to create innovative new technologies
- Pediatric subspecialists: an MFM bound resident elected to rotate through pediatric subspecialty clinics to gain insight and experience with how to counsel parents about fetal anomalies and neonatal treatment options.
- Community Outreach: many residents have spent time working in community substance abuse programs, complex family planning centers, and volunteer experiences.
- Research: residents can dedicate time on tracking to pursue research endeavors
Curriculum
PGY-1
During the first year, residents expand their clinical knowledge across a broad range of topics in obstetrics and gynecology. They are introduced to a variety of practice settings and subspecialties, providing early exposure to potential career paths.
- Gynecologic Oncology (6 weeks)
- Fairview OB Days (6 weeks)
- Fairview OB Nights (6 weeks)
- Benign Gynecology (6 weeks)
- Fairview OBGyn Hospitalist (3 weeks)
- Outpatient/Evidence-Based Medicine (3 weeks)
- Midwifery/Postpartum Care (3 weeks)
- SICU (3 weeks)
- Main Campus Gyn Nights (3 weeks)
- Hillcrest ObGyn Hospitalist (3 weeks)
- TRACKING (3 weeks)
| Fall | Spring |
| Gyn Onc | Gyn Onc |
| Fairview OB | Fairview OB |
| Fairview Nights | Fairview Nights |
| Benign Gyn | Benign Gyn |
| Fairview ObGH | Tracking |
| Outpatient/EBM | SICU |
| US/Quality | Main Campus Nights |
| Midwife/PP | Hillcrest ObGH |
PGY-2
During the second year, residents engage more deeply with advanced topics in obstetrics and gynecology. They begin applying their knowledge to increasingly complex and nuanced clinical situation, developing critical thinking and decision-making skills. This stage of training builds on foundational learning and supports continued progression toward independent, well-rounded clinical practice.
- Gynecologic Oncology (6 weeks)
- Fairview OB Days (6 weeks)
- Fairview OB Nights (3 weeks)
- Main Campus Gyn Nights (3 weeks)
- Benign Gynecology (6 weeks)
- Family Planning
- Hillcrest Antepartum/MFM
- MIGS (3 weeks)
- Urogyn/URPS (3 weeks)
- TRACKING (6 weeks)
| Fall | Spring |
| Gyn Onc | Gyn Onc |
| Fairview OB | Fairview Days |
| Main Campus Nights | Fairview Nights |
| Benign Gyn | Benign Gyn |
| Tracking | Tracking |
| Family Planning | MIGS |
| Hillcrest Ante/MFM | Urogyn/URPS |
PGY-3
During the third year, residents take on greater responsibility in managing complex clinical scenarios across obstetrics and gynecology. They refine their clinical judgment, broaden their surgical skills, and begin to function with increased autonomy in both inpatient and outpatient settings. PGY3-residents also play a key leadership role by supervising junior learners and stepping up as the leader of the L&D and antepartum team in the Spring.
- Gynecologic Oncology (6 weeks)
- Fairview OB Days (6 weeks)
- Fairview OB Nights (6 weeks)
- Benign Gynecology (6 weeks)
- Main Campus GYN Nights (3 weeks)
- Hillcrest Antenatal/MFM (3 weeks)
- Urogyn/URPS (3 weeks)
- Reproductive Endocrinology (3 weeks)
- TRACKING (6 weeks)
| Fall | Spring |
| Gyn Onc | Gyn Onc |
| Fairview Days | Fairview Days |
| Fairview Nights | Fairview Nights |
| Benign GYN | Benign GYN |
| Tracking | Tracking |
| Main Campus Nights | REI |
| Urogyn/URPS | Hillcrest Ante/MFM |
PGY-4
By the fourth year, residents demonstrate advanced proficiency in clinical care, surgical skills, and leadership. They function with a high degree of autonomy and efficiency, preparing for independent practice or fellowship training. As chief or senior residents, they lead teams, mentor junior learners, and model professionalism and sound clinical judgment. This final year consolidates their knowledge and skills to ensure they are confident competent, and practice ready.
- Gynecologic Oncology (6 weeks)
- Fairview OB Days (6 weeks)
- Fairview OB Nights (3 weeks)
- Benign Gynecology (6 weeks)
- Hillcrest Antenatal/MFM (3 weeks)
- Hillcrest OBGYN Hospitalist (3 weeks)
- Fairview OBGYN Hospitalist (3 weeks)
- Continuity Clinic Chief (3 weeks)
- Float/GYN Surgery (6 weeks)
- TRACKING (6 weeks)
| Fall | Spring |
| Gyn Onc | Gyn Onc |
| Fairview OB | Fairview OB |
| Fairview Nights | Main Campus Nights |
| Benign Gyn | Benign GYN |
| Tracking | Tracking |
| Hillcrest Ante/MFM | Continuity Clinic Chief |
| Hillcrest ObGH | Fairview ObGH |
| Float/Gyn Surgery | Float/Gyn Surgery |
View the specific outcomes plan.
Rotation Details
Obstetrics Residents have the opportunities to be involved with obstetrical patients at each of our regional hospitals, Hillcrest and Fairview along with Main Campus. Our regional hospitals' labor and deliver units each do between 4,500-5,000 deliveries per year. Our patient population at each of these hospitals offers residents the opportunities to care for patients of all backgrounds. Residents work on teams with varied levels of responsibility based on post graduate year and are involved in all aspects of obstetrical care. Residents manage patients on antepartum, intrapartum and postpartum. Vaginal Deliveries, VAVD, FAVD, primary and repeat cesarean section are typical procedures residents learn as they master basic and then more complicated obstetrical situations. In addition to managing faculty obstetrical patients, residents also deliver their patients from the continuity Westown Clinic at Fairview Hospital.
The Maternal Fetal Medicine rotations takes place at Hillcrest and Fairview Hospitals. During the second year the rotation is primarily an outpatient consultation and ultrasound experience where residents work directly with clinical faculty. The third year rotation is primarily an inpatient rotation where residents manage the antepartum service and perform complicated obstetrical surgeries under the supervision of the Maternal Fetal Medicine faculty as well as spending time in the outpatient office learning ultrasound, genetics and consultation.
The Gynecology rotation occurs in each of the four years with residents operating as early as their first year. Residents are involved in level-appropriate cases that are assigned by the gynecological chief resident. This gives the chief residents the autonomy needed to develop into supervising physicians as well as to select the most valuable clinical experiences for the resident teams
Residents have the opportunity to participate in cases at various sites allowing for a vast surgical experience. They operate with our specialty (general) OBGYN surgeons along with our Minimally Invasive Gynecologic Surgical team performing cases that vary in complexity from simple to advanced. Residents typically graduate with well over double the minimal required cases in many categories. Residents have 24/7 access to a dry simulation lab to master their laparoscopic and hysteroscopic skills even prior to entering the operating room.
On Gynecologic Oncology the resident team learns the care of acute and chronically ill patients. Clinical management begins in the first year with progressive involvement in complex surgical cases. Residents work with the staff and fellows on this rotation to evaluate patients with female cancers in outpatient clinics and are involved in their surgical procedures and perioperative management. Our nationally recognized gynecologic oncologists perform innovative approaches to surgery with a focus on minimally invasive surgery. Residents participate in open surgeries, laparoscopic and single port laparoscopies. Cleveland Clinic values a culture where all individuals feel valued and included. We respect and appreciate our similarities and differences; they enable us to better serve our patients, one another and our global communities.
Female Pelvic Medicine and Reproductive Surgery: Residents will become familiar with the surgical management of pelvic floor disorders. Surgical skills like vaginal hysterectomy, vaginal suspension procedures and midurethral sling placement are the focus of the urogynecology rotation. Nationally recognized staff educate our residents about a wide variety of diagnoses including pelvic organ prolapse and urinary incontinence.
Reproductive Endocrinology and Infertility will allow residents to evaluate complex infertility issues and patients with endocrine challenges. This rotation also provides the opportunity to work with national leaders in endometriosis who are exploring innovations in endometriosis imaging. Advanced laparoscopic surgeries are utilized to treat patients with tubal disease, endometriosis and pelvic pain.
Ultrasound Training is comprehensive ranging from Obstetrical to Gynecologic sonograms and saline infusion sonography. Residents get a robust experience in the outpatient clinical offices, didactic experience, high risk clinics and family planning rotation. Advanced simulation equipment in available and residents also have a first year rotation completely dedicated to ultrasonography.
The Family Planning rotation is a Kenneth J. Ryan Residency Training Program. The program is part of a national initiative to enhance comprehensive resident training in uterine evacuation techniques, complex contraception, LARC, and grieving/bereavement counseling. Our program has been carefully designed to be in full compliance with all ACGME requirements and maintains a partial participation option for our residents.
Global Health (tracking opportunity) experiences with Dr. Miriam Cremer, Cleveland Clinic Staff Physician and President/Founder of Basic Health International gives the residents opportunities to become involved in global health.
Cervical cancer is the leading cause of cancer death in many developing Cervical Cancer Prevention Program (CAPE) is a pilot program with the Salvadoran Ministers of Health in El Salvador. Over 30,000 were screened through this program which not only established an infrastructure for a sustained system of cervical cancer prevention in El Salvador; but also created the framework for a viable model of replication in resource-poor countries. The program mission is to eradicate cervical cancer globally. Dr. Cremer and BHI are also involved in a project to introduce HPV DNA based screening in Haiti. Through the Cleveland Clinic, Dr. Cremer is PI on several NIH research projects working to develop an inexpensive, mobile, effective treatment device for cervical pre-cancer.
Education and Simulation
-
-
-
-
-
-
2019 Residency Team building and Simulation Event | Cleveland Clinic
-
-
Didactics
Every Wednesday morning residents have four hours of protected didactic time. Education during this time includes Grand Rounds, Didactics, Morbidity and Mortality Conference, Journal Club, Ultrasound Conference, Quality Updates, and Simulation.
Educational activities are monitored through semi-annual program reviews, rotation-by-rotation specific feedback, program surveys and attendance at conferences, rounds and journal clubs. The education team is a multi-disciplinary team involving residents, staff, administrative support, graduate medical education support and many more members invested in resident education.
In addition to scheduled didactics, structured learning occurs on clinical services with supervising attending physicians and subspecialty fellows.
Simulation
State-of-the-Art Simulation Center
Cleveland Clinic’s Education Institute multidisciplinary simulation center is designed to enhance the clinical learning experience for healthcare professionals. All physicians, nurses and allied health providers can engage in high-fidelity, team-based interventions to learn specific clinical skills or to practice new technical skills such as laparoscopy through the use of state-of-the-art task simulators. The Simulation Center provides an interactive learning experience in a low-stress, risk-free environment.
Scheduled Simulation
The first Wednesday of every month is dedicated to resident simulation. This alternates between obstetrical and gynecological experiences. Examples of simulations include laparoscopy, robotic training, complex perineal repairs, emergency cesarean section, obstetrical hemorrhage, and cadaveric dissections. Our Minimally Invasive Gynecologic Surgeons are dedicated to facilitating both low and high fidelity simulation scenarios. We also have faculty who have done fellowship training in simulation who help to create robust experiences for all level residents. Simulation is paired with didactics to maximize resident learning and engagement.
Residents typically complete their Fundamentals of Laparoscopic Surgery within their first year.
Residents have the opportunity to participate in a structured robotic training curriculum that spans all four years of training. This curriculum incorporates participation in the Robotic Training Network, and includes completion of online modules, simulation tasks, didactics, small group simulation labs, hands-on operative training and faculty assessment. The program emphasizes proficiency-based advancement of skills, providing experience to bedside assist and basic surgical skills for the robotic platform. Those with an interest may also opt to pursue advanced training during tracking block.
Intern Bootcamp
Each year in July, we start out the year with seven weeks of introductory simulations to introduce our Interns to basic surgical skills. Facilitated by faculty and PGY-3 residents, interns learn: knot tying, suturing, anatomy, laparoscopy and vaginal deliveries (spontaneous, vacuum, and forceps), cesarean sections and perineal repairs. This allows clinical skill development along with the opportunity for the new intern class to development relationships amongst themselves and with upper level residents.
Skill Based Team Building
A team building surgical skill experience in July is just the beginning of the simulation program our residents experience. This event allows senior residents to guide junior residents through various simulations in a fun interactive environment. Examples of these activities include simulated cerclage placement, circumcisions, laparoscopic treasure hunts, patwardhan technique, surgical positioning, laparoscopic led signatures, amniocentesis, post-partum hemorrhage devices, forceps, I-Pass, and IUD placement.
In the spring the annual resident Olympics provide opportunities for skill development and resident well-being in addition to mock oral board exams. Examples include OBGYN escape room, pessary toss and endometrial biopsy relays.
Our staff physicians are engaged highly at each of these simulation to coach and mentor residents throughout the experiences. Staff can even be spotted during our Olympic opening ceremonies caring their iPhone flashlights as torches.
Research
Research Opportunities
Every year celebrate research in the Obstetrics and Gynecology Institute with our Resident Research Day. Third year residents give oral podium presentations on their research while second year residents present posters highlighting their projects. In addition, residents consistently present their research at other local and national meetings.
Faculty provide mentorship throughout the research and publication process. Our faculty research is recognized nationally through publications, national academic leadership positions and extensive grant funding.
To help support research endeavors, the Obstetrics and Gynecology Institute has six full-time and two part-time research staff including five RN research nurse coordinators, three non-RN research coordinators and an RN nurse manager. The clinical research team is responsible for all patient-related aspects of your research project with respect to regulatory compliance.
Hospital and Clinic Locations
Hospitals
Cleveland Clinic provides patient care for regional, national and international patients at locations throughout the Cleveland metropolitan area. Most training will take place at Cleveland Clinic’s main campus. Residents will also train at Fairview and Hillcrest hospitals, both of which are Cleveland Clinic hospitals that provide general and high-risk obstetrics care as well as general and sub-specialty surgical care.
In addition, the resident outpatient continuity clinic will take place at Westown Physician’s Center which is located near Fairview Hospital. This is a resident run clinic staffed by 25 staff physicians that have training and interest in outpatient clinical teaching.
Additionally:
- Founded in 1921 by George Crile Sr.
- 44 buildings, over 85 operating rooms, more than 1,400 beds.
- Special Delivery Unit focuses on delivery of women or infants who will require special monitoring and/or interventions around or after delivery.
- Fairview Hospital is a busy 488 bed community hospital on Cleveland’s west side overlooking the city's Metro parks.
- Features a Level III NICU, and a Level II Trauma Center.
- Over 5,000 deliveries per year.
- Features the Fairview Family Birth Place, a low intervention birthing unit.
- Baby-Friendly designation.
- Hillcrest Hospital is a busy 500 bed community hospital located on the east side of Cleveland.
- Hillcrest Hospital features a level III NICU and level II trauma center.
- Over 4,000 deliveries per year.
- Features OB Emergency Department and low intervention birthing suites.
Ambulatory Surgery Centers
Westown Continuity Clinic
- Located 10 minutes from Fairview Hospital.
- On-site pediatrics, internal medicine, social service and county WIC services.
- Resident-led Centering OB visits offered.
Current Residents
Class of 2026

Megan Ansbro, MD, PhD
- Undergraduate: Denison University
- Medical School: University of California, Irvine, School of Medicine

Dana Baraki, MD
- Undergraduate: The College of William and Mary Williamsburg
- Medical School: Eastern Virginia Medical School

Parker Bussies, MD
- Undergraduate: Hope College – Holland, MI
- Medical School: University of Miami - Leonard M. Miller School of Medicine

Andreea Dinicu, MD
- Undergraduate: University of Connecticut
- Medical School: University of California, Irvine, School of Medicine

Emma Gargus, MD, PhD
- Undergraduate: Massachusetts Institute of Technology
- Medical School: Northwestern University The Feinberg School of Medicine

Marissa Hand, MD
- Undergraduate: University of Virginia
- Medical School: Georgetown University School of Medicine

Jennifer Hansen, MD
- Undergraduate: Johns Hopkins University Krieger School of Arts and Sciences
- Medical School: Frank H. Netter MD School of Medicine at Quinnipiac University

Sunny Lee, DO
- Undergraduate: Purdue University
- Medical School: Kansas City University College of Osteopathic Medicine
Class of 2027

Rachel Cevigney, MD
- Undergraduate: University of Michigan
- Medical School: Wayne State University School of Medicine

Cameron Harris, MD
- Undergraduate: University of North Carolina at Chapel Hill
- Medical School: University of North Carolina at Chapel Hill School of Medicine

Chloe Kaunitz , DO
- Undergraduate: University of Pittsburgh
- Medical School: Chicago College of Osteopathic Medicine of Midwestern University

Alexandra McKinzie, MD
- Undergraduate: Indiana University
- Medical School: Indiana University School of Medicine

Gabrielle Mintz, MD
- Undergraduate: Vassar College
- Medical School: University of Arizona College of Medicine – Tucson

Rachel O’Brien, MD
- Undergraduate: University of California, Los Angeles
- Medical School: University of Virginia School of Medicine

Ariella Yazdani, MD
- Undergraduate: Union College, Schenectady
- Medical School: Robert Larner, M.D., College of Medicine at the University of Vermont
Class of 2028

Cydni Akesson, MD
- Undergraduate: Case Western Reserve University
- Medical School: Cleveland Clinic Lerner College of Medicine

Julie Chugh, MD
- Undergraduate: The University of Texas
- Medical School: Texas Tech University Health Sciences School of Medicine

Emily Ho, MD, PhD
- Undergraduate: University of Chicago
- Medical School: University of California, San Diego, School of Medicine

Elizabeth Klein, MD
- Undergraduate: Cornell University
- Medical School: The Warren Alpert Medical School of Brown University

Sara Koussa, MD
- Undergraduate: Allegheny College
- Medical School: Wayne State University School of Medicine

Margo Nelis, MD
- Undergraduate: The Ohio State University
- Medical School: University of Kentucky College of Medicine

Caleigh Smith, MD
- Undergraduate: Duke University
- Medical School: University of Virginia School of Medicine
Class of 2029

Amrita Ladwa
- Medical School: University of Virginia

Emily Martinbianco
- Medical School: Loyola of Chicago Stritch School of Medicine

Madison McCracken
- Medical School: Anne Burnett Marion School of Medicine at TCU

Jameson Mitchell
- Medical School: Cleveland Clinic Lerner College of Medicine of Case Western Reserve

Stevie Muscarella
- Medical School: Pennsylvania State University College of Medicine

Elizabeth Stanley
- Medical School: Cleveland Clinic Lerner College of Medicine of Case Western Reserve

Megan Wasson
- Medical School: Emory University School of Medicine

Morgan Yapundich
- Medical School: Wake Forest University School of Medicine
Staff
Staff Obstetrics and Gynecology and Women's Health Institute
Cleveland Clinic caregivers are involved in clinical innovations that are advancing the care of women and the field of Obstetrics and Gynecology. Some of these advances are highlighted in the following Cleveland Clinic OB/GYN and Women’s Health Institute publications and news releases:
Publications:
News releases:
- Cleveland Clinic Receives $2 Million Gift to Establish First Endowed Chair for Uterine Cancer Research
- Cleveland Clinic First in North America to Deliver Baby from Deceased-Donor Uterine Transplant
- Cleveland Clinic Performs Its First In Utero Fetal Surgery
Research, insights and innovations:
- Obstetrics Emergency Department Caters to Unique Needs of Expectant Parents
- Doula Program Improves the Birthing Experience and Patient Outcomes
- Novel Medications Boost Treatment Options for Patients With Postpartum Depression
- Experienced Specialists Team Up for Complex Surgical Obstetrics
- Cleveland Clinic Launches Center for Infant and Maternal Health
Academic Appointments
Cleveland Clinic Lerner College of Medicine, Case Western Reserve University
- Marjan Attaran, MD, Clinical Assistant Professor of Surgery, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Stephen Bacak, DO, MPH Clinical Assistant Professor
- Rebecca Bagley, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Fadi Bashour, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Pelin Batur, MD, Associate Professor
- Lauren Bouchard, MD, Clinical Assistant Professor
- Natalie Bowersox, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Linda Bradley, MD, Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Amy Burkett, MD, Clinical Assistant Professor
- Jeffrey Chapa, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Anna Chichura, MD, Clinical Instructor
- Edward Chien, MD, MBA Professor
- Francine Cosner, MD, Clinical Assistant Professor
- Miriam Cremer, MD, MPH, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Robert DeBernardo, MD, Associate Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Brittany Denny, DO, Clinical Assistant Professor
- Jillian Dodge, DO, Clinical Assistant Professor
- Meredith Dorr, MD, Clinical Assistant Professor
- Kenneth Edelman, MD, Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Ashraf El-Dabh MD, Clinical Assistant Professor
- Jonathan Emery, MD, Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Tommaso Falcone, MD, Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Lourdes Falconi, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Ruth Farrell, MD, Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Amanda Ferry, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Jonathan Funk, MD, Clinical Assistant Professor
- Julia Girzhel, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Oluwatosin Goje, MD Associate Professor
- Jeffrey Goldberg, MD, Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Rhoda Goldschmidt, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Erin Higgins, MD, Clinical Assistant Professor
- Maeve Hopkins, MD, Clinical Assistant Professor
- Patrick Isaac, DO, Clinical Assistant Professor
- Joan Jesse, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Stacie Jhaveri, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Sarah Juza, MD, Clinical Assistant Professor
- Amanda Kalan, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Monique Katsuki, MD, Assistant Professor
- Fadi Khoury, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Melissa Kirven, MD, Clinical Assistant Professor
- Swapna Kollikonda, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Suchetha Kshettry, MD, Clinical Assistant Professor
- Mary LaPlante, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Justin Lappen, MD, Associate Professor
- Melissa Lee, MD, Clinical Assistant Professor
- Hanna Lisbona, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Erin McKelvey, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Margaret McKenzie, MD, Associate Professor
- Gita Mehta, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Amy Merlino, MD, Assistant Professor
- Chad Michener, MD, Associate Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Sharon Mikol, MD, Clinical Assistant Professor of Surgery, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Trina Pagano, MD, Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Marie Paraiso, MD, Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Betsy Patterson, MD, Clinical Assistant Professo, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Uma Perni, MD, MPH, Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Kim Puterbaugh, MD, Clinical Assistant Professor
- Sudhakar Rao, MD, Clinical Assistant Professor
- Vicki Reed, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Mitchell Reider, MD, Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Jean Reinhold, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Stephanie Ricci, MD, Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Beri Ridgeway, MD, Academic Department Chair, Associate Professor
- Peter Rose, MD, Professor
- Rebecca Russell, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Sabrina Sahni, MD, Clinical Assistant Professor
- Abdelaziz Saleh, MD, Clinical Professor
- Alexis Scaparotti, MD, Clinical Assistant Professor
- Maria Schleicher, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Lynn Simpson, MD, Clinical Assistant Professor
- Katherine Singh, MD, Assistant Professor
- Amber Somerville, MD, Clinical Assistant Professor
- Amy Stephens, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Womack Stokes, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Jessica Strasburg, MD, Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Sharon Sutherland, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Monica Svets, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Holly Thacker, MD, Professor, Ob/Gyn & Women’s Health Institute, Center for Specialized Women’s Health
- Tonya Thomas, MD, Clinical Assistant Professor
- Roberto Vargas, MD, Clinical Assistant Professor
- Mark Walters, MD, Professor
- Catherine Wilkins, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Diane Young, MD, Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
- Salena Zanotti, MD, Clinical Assistant Professor, Ob/Gyn & Women’s Health Institute, Ob/Gyn
Alumni
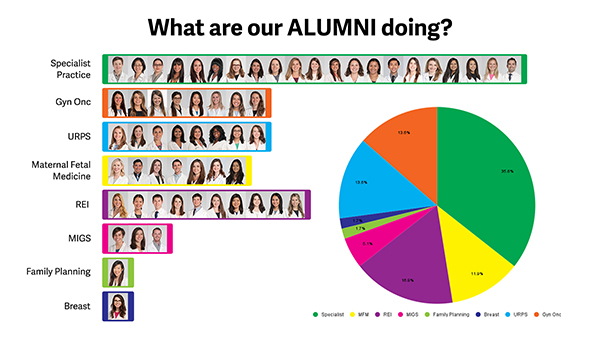
Cleveland Clinic Obstetrics & Gynecology Residency Program Alumni
| 2025 | Emily Armstrong, MD | Ob/Gyn Staff, Cleveland Clinic, Cleveland, OH |
| 2025 | Riva Desai, MD | Ob/Gyn Staff, Cleveland Clinic, Cleveland, OH |
| 2025 | Katarina Fleckenstein, MD | Ob/Gyn Staff, St. Joseph’s Chandler, Savannah, GA |
| 2025 | Olivia Neumann, MD | Ob/Gyn Staff, Cleveland Clinic-Avon Pointe, Avon, OH |
| 2025 | Emily Frisch, MD | REI Fellowship at Stanford University, Stanford, CA |
| 2025 | Kirat Sandhu, MD | MFM fellowship at University Hospital/Case Western Reserve |
| 2025 | Dominic Sandler, MD | Ob/Gyn Staff, Cleveland Clinic, Cleveland, OH |
| 2024 | Sabrina Bains, MD | REI Fellowship, Weill Cornell Medicine, New York, NY |
| 2024 | Lauren Buckley, MD | MFM Fellowship, Vanderbilt University |
| 2024 | Katie Klammer, MD | MFM Fellowship, University of Pennsylvania Medicine |
| 2024 | Erika Lampert, MD | Gynecologic Oncology Fellowship, University of Pittsburgh Medical Center – Magee |
| 2024 | Madeline Lederer, MD | Ob/Gyn Private Practice, Northwestern Specialists for Women, Chicago, IL |
| 2024 | Johnathan Zhao, MD | Ob/Gyn Staff, Clinica Sierra, Fresno, CA |
| 2023 | Rachael Baird, MD, MS | Faculty, Advocate Aurora BayCare Medicine Center, Green Bay, WI |
| 2023 | Julia Chalif, MD | Gynecologic Oncology Fellowship, The Ohio State University |
| 2023 | Alexandra Imani Chatman, MD | Faculty, Cleveland Clinic |
| 2023 | Catherine Keller, MD | Academic Generalist, Carle Foundation Hospital, Carlisle, PA |
| 2023 | Kaia Schwartz, MD | Reproductive Endocrinology and Infertility Fellowship, University of California, San Francisco |
| 2023 | Rachel Shin, MD, MPH | Complex Family Planning Fellowship, Oregon Health & Science |
| 2023 | Annika Sinha, MD | Female Pelvic Medicine and Reconstructive Surgery Fellowship, Duke University |
| 2023 | Nicole Wood, MD | Female Pelvic Medicine and Reconstructive Surgery Fellowship, Hartford Hospital |
| 2022 | Carrie Bennett, MD | MFM Fellowship, University of Pittsburgh Medical Center Magee - Women's Hospital |
| 2022 | Jonathan T. Hunt, MD, MBA | Faculty, Naval Medical Center, Portsmouth |
| 2022 | Ukpebo Rebecca Omosigho, MD | Female Pelvic Medicine & Reconstructive Surgery Fellowship, Vanderbilt University |
| 2022 | Morgan Gruner, MD | Gynecologic Oncology Fellowship, University of Minnesota |
| 2022 | Mary Kate Lintel, MD | Ob/Gyn Specialist, Wellstar, Atlanta, GA |
| 2022 | Cory Messingschlager, MD | Minimally Invasive Gynecologic Surgery Fellowship, University of Tennessee College of Medicine |
| 2022 | Molly Morton, MD | Gynecologic Oncology Fellowship, The Ohio State University |
| 2021 | Anna Chichura, MD | Breast Surgical Oncology Fellowship Program at North Shore and the University of Chicago Medicine |
| 2021 | Alyssa Herrmann, MD | Ob/Gyn Specialist, Private Practice - Eastside Gynecology and Obstetrics as an Ob/Gyn specialist in Detroit, Michigan |
| 2021 | Melanie Katz, MD | Faculty, Cleveland Clinic |
| 2021 | Lia Miceli, MD | FPMRS Fellowship, Methodist Hospital-Houston-TX Pelvic Medicine and Reconstructive Surgery OBGYN-Houston, TX |
| 2021 | Ji “Jessica” Son, MD | Gynecologic Oncology Fellowship, Univ of TX, MD Anderson, Houston, TX |
| 2020 | Deepanjana Das, MD | FPMRS, Fellowship - Northwestern McGaw Medical Center |
| 2020 | Sarah Hershman, MD | Faculty, Obstetrics & Gynecology, Cleveland Clinic |
| 2020 | Emily Holthaus, MD | MFM Fellowship, Loyola University Medical Center |
| 2020 | Christine Hur, MD | REI Fellowship, Cleveland Clinic |
| 2020 | Erica Newlin, MD | Faculty, Obstetrics & Gynecology, Cleveland Clinic |
| 2019 | Caitlin Carr, MD | Gynecologic Oncology Fellowship – Mount Sinai Hospital |
| 2019 | Chelsea Fortin, MD | REI Fellowship – University of Michigan |
| 2019 | Julian Gingold, MD, PhD | REI Fellowship – Albert Einstein College of Medicine, Montefiore Medical Center |
| 2019 | Natalia Llarena, MD | REI Fellowship – Cleveland Clinic |
| 2019 | Jessian Munoz, MD, PhD | MFM Fellowship – University of Texas, San Antonio |
| 2019 | Kate Woodburn, MD | FPMRS Fellowship – MedStar Washington Hospital Center – Georgetown University |
| 2018 | Alexander Kotylar, MD | REI Fellowship - Yale University, New Haven, CT |
| 2018 | Thanh Ha Luu | REI Fellowship - University of Colorado, Denver, CO |
| 2018 | Laura Moulton, DO | Gynecologic Oncology Fellowship - Cleveland Clinic, Cleveland, OH |
| 2018 | Emily Nacy, MD | Assistant Professor, Division of General Obstetrics and Gynecology - University of Utah, Salt Lake City, UT |
| 2018 | Sarah Steele, MD | FPMRS Fellowship - University of California, Irvine, CA |
| 2017 | Chiazor Akusoba, MD | Private Practice, Washington |
| 2017 | Cynthia Arviso, MD | MIS Fellowship - Vanderbilt, Nashville, TN |
| 2017 | Lisa Hickman, MD | FPMRS Fellowship - Cleveland Clinic |
| 2017 | Suejin Kim, MD | Private Practice, California |
| 2017 | Lindsay Valentine, MD | MIS Fellowship - Penn State, Hershey, PA |
| 2016 | Melanie Arora, MD | Private Practice, Apple Valley, CA |
| 2016 | Megan Buechel, MD | Gynecologic Oncology Fellowship University of Oklahoma, Oklahoma City, OK |
| 2016 | Ginny Marie Harris, MD, PhD | Private Practice |
| 2016 | Monique Katsuki, MD | Faculty, Obstetrics & Gynecology Cleveland Clinic |
| 2016 | Jamie Stanhiser, MD | Reproductive Endocrinology & Infertility Fellowship University of North Carolina Chapel Hill, NC |
Resident Life
Our program emphasizes the health and well-being our residents. We have developed a “L.E.A.D.E.R” Series that focuses on Leadership, Equanimity, Acceptance, Diversity, Engagement and Resilience throughout the residency. Through this program’s curriculum, we have focused on team building, mentorship with staff/colleagues, mindfulness, professionalism and leadership development. To this: We focus on team building, mentorship with staff/colleagues, mindfulness, professionalism and leadership development.
Resident Retreat
Each fall, the residents participate in a resident only retreat. This is an opportunity for residents to get to know one another on a more personal level, spend time together outside of the hospital setting, participate in team building activities and have discussions on ways to continue to improve and strengthen the training program. The retreat is fully supported by the administration and the current fellows. All residents participate and are excused from clinical activities and responsibilities during this time.
Ryan Program
Cleveland Clinic's Obstetrical and Gynecological Institute and Ob/Gyn Residency Program are dedicated to providing comprehensive Complex Family Planning training.
We are a training site for the Kenneth J. Ryan Residency Training Program, which is a national initiative that offers Complex Family Planning training for residents in Obstetrics and Gynecology through education, evidence-based clinical training and research in academic medical settings.
Application Process
The Obstetrics and Gynecology Institute offers 8 categorical residency positions each year. Currently there are a total of 30 categorical residents in the program. This is an increase in 3 positions from the 5 since 2017. Currently there are a total of 30 categorical residents in the program. All positions are filled through the National Residency Matching Program (NRMP). No preliminary (PGY1) or advanced positions (PGY2) are offered through the Match. International applicants are invited to apply through the ERAS and participate in the NRMP as well.
How to Apply
The Ob/Gyn Residency Program participates in ResidencyCAS for all positions. You must complete all components of the ResidencyCAS in order for your application to be considered complete and to be reviewed by the Selection Committee. Our supplemental requirements include three letters of recommendation and all COMLEX and USMLE scores must be included in your application.
- Complete Application.
- CV.
- Personal Statement.
- Medical Student Performance Evaluation (MSPE).
- Medical School Transcript.
- USMLE Step I Transcript & Score Report – must pass one your first attempt.
- USMLE Step 2 Transcript & Score Report – must pass one your first attempt.
- Must have USMLE Step 2 Score Report uploaded into ERAS prior to the deadline of the Rank List submission. If you do not have a Step 2 Score Report uploaded, you will not be ranked (assuming you were invited for an interview).
- Three Letters of Recommendation.
International Medical Graduates
Here are some frequently asked question by graduates of international medical schools regarding the application process:
- ECFMG certification at the time of application is required. Please review the ECFMG requirements for additional information.
- Must have graduated medical school within the last 5 years. Anything greater than 5 years does not meet the minimum requirements.
Application Deadline
September 24, 2025.
Interviews
Offers for interviews will be made starting on October 28, 2025, according to CREOG/APGO guidelines. 2025-2026 interviews will be held virtually.
Please take a moment to watch this video, which will help outline the world class training you can receive at Cleveland Clinic.
Life in Cleveland has so much to offer! Learn more about the city of Cleveland.
For more information:
Erin Hodgson
Residency Program Manager
216.445.5125
hodgsoe@ccf.org
Benefits
Benefits Overview
Approved Time Off
15 vacation days and 5 personal days are provided at the beginning of each academic year.
Insurance
All clinical trainees at Cleveland Clinic receive medical, dental, vision, prescription, life, and short-term disability insurance coverage. Medical insurance is provided with a small premium paid by the resident. Insurance covers residents and their families fully and is effective on the first day of training with no waiting period.
Educational Allowance
Each resident will receive $500 per academic year to use for educational purchases and reimbursement. This can be used for books, tablets, laptops, society dues, etc. In addition, it can be used to offset the cost of the USMLE Step 3 exam. Residents can also choose to use this amount as a lump sum.
The Education Institute (GME Department will fund up to $2,500 per year for meeting attendance for PGY Year 2 and above that have an abstract or poster accepted for presentation at a national meeting. Additional funding for travel and meeting attendance is available through the Obstetrics and Gynecology Institute pending an approval process. Meeting attendance does not subtract from vacation days.
Salary
Please refer to the table below for new salary rates, effective May 16, 2024:
| Grad Level | New Annual Rate | New Per Pay Rate |
|---|---|---|
| 1 | $67,322 | $2,805 |
| 2 | $69,591 | $2,900 |
| 3 | $71,838 | $2,993 |
| 4 | $74,649 | $3,110 |
| 5 | $77,137 | $3,214 |
| 6 | $80,171 | $3,340 |
| 7 | $82,826 | $3,451 |
| 8 | $84,441 | $3,518 |
| 9 | $86,063 | $3,586 |
| 10 | $88,405 | $3,684 |
Additional Benefits
- Additional information regarding benefits can be viewed on the GME website