Compression Stockings
(also known as Thrombo-Embolic Deterrent or T.E.D. stockings, anti-embolic stockings or graduated pressure stockings)
If you have had surgery or are at risk for a DVT, you may be prescribed compression stockings when you return home. These stockings help:
- Promote return of blood in the blood vessels (veins to the heart).
- Prevent blood from pooling in the legs and causing blood clots.
Compression stockings are tight fitting stockings that are tight at the ankle and become looser as they go up the leg. This causes gentle external compression (or pressure) on your leg.
Most compression stockings are worn just below the knee, although there are thigh-high stockings that are sometimes prescribed. If you are wearing compression stockings, they should feel snug but not too tight.
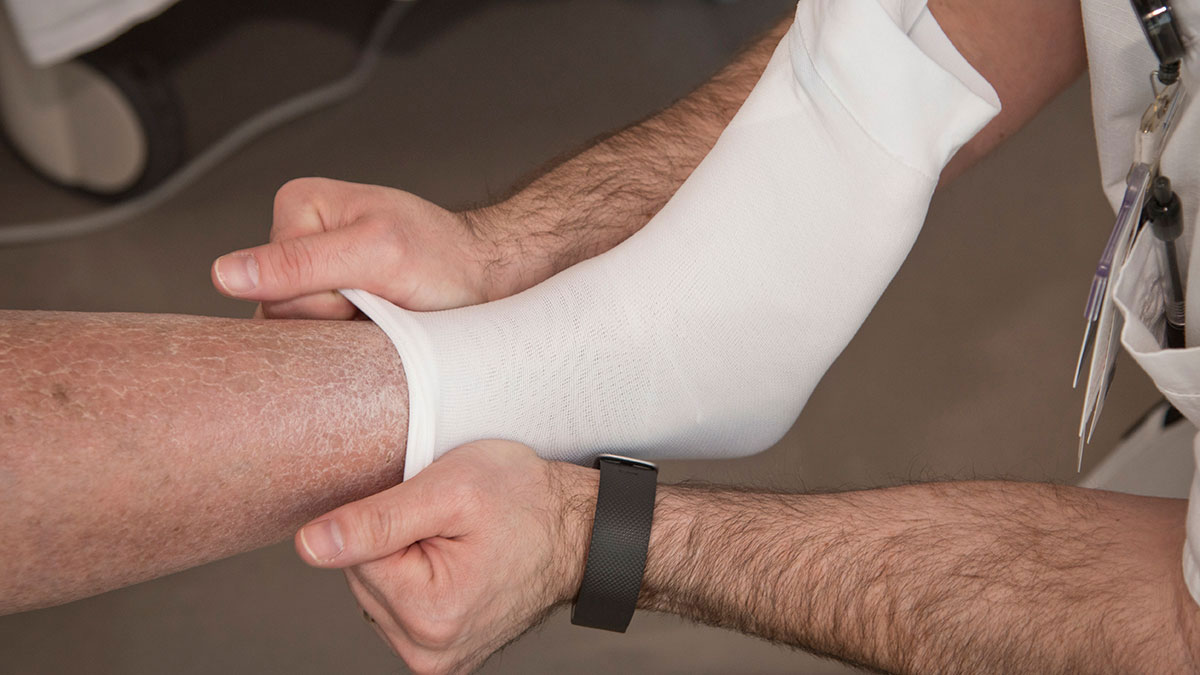
How to put on Compression Stockings
1 of 6-
1. Unwrap the stockings so that the heel and toe are in the same direction as your foot.
-
2. Start putting on the stockings at the lower ankle first. The ankle will have the most pressure and therefore will be the most difficult to place. (Some people find it helpful to put their hand in the stocking and turn it inside out at the ankle to put that part of the sock on first).
-
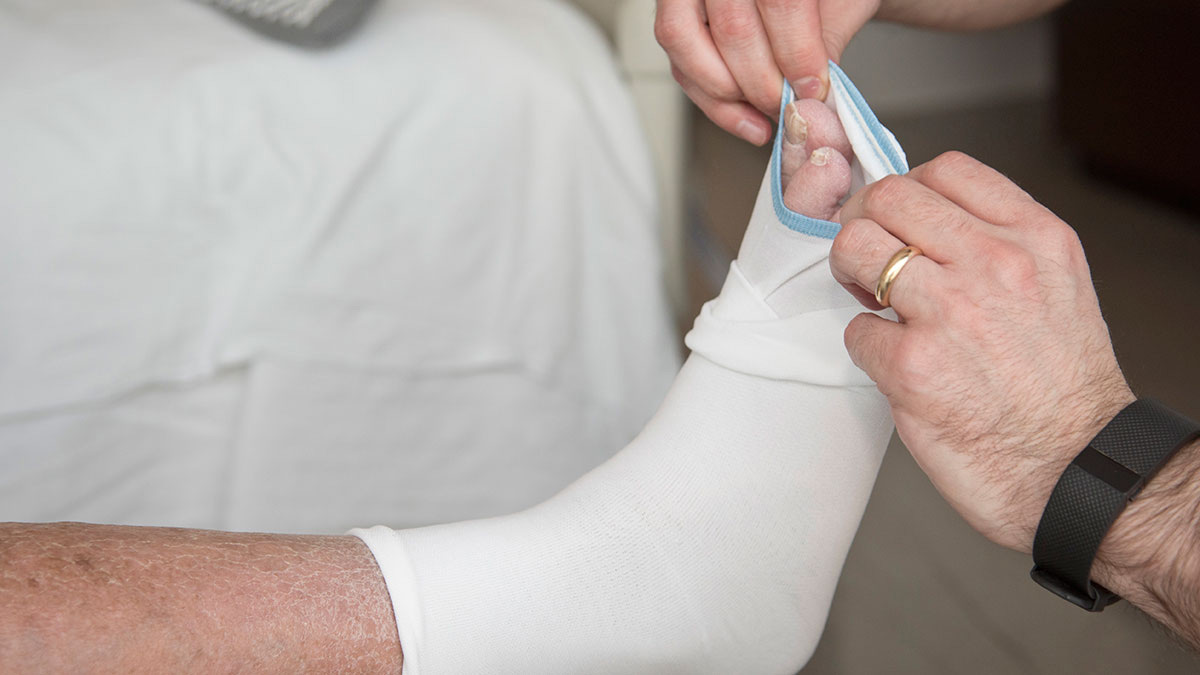
3. Make sure the toe and heel is in the right place on the foot.
-
4. Pull the stocking up the leg.
-
5. Make sure the stocking is lying evenly on the leg. Smooth out any rolls. Avoid any bunching or uneven stockings. The stocking should be below the knee. Make sure they are not too long. Never turn the tops of the stockings over as that will lead to a tourniquet like effect.
-
6. You may feel more comfortable with socks or slippers over the stocking. It is ok to wear socks, slippers or shoes over your compression stockings.
Note: Patients who have difficulty putting on their TED stockings, may require assistance from someone or there are assist devices to help patients put on the stockings to make sure the heel is in place and includes grips to limit bending.
Frequently asked questions about compression stockings
How do I clean the stockings?
Stockings may be washed by hand and hung to dry. They may also be machine washed and dried according to package instructions using low heat. Do not use bleach.
How long do I wear the stockings?
- You should wear them as much as possible. You may take them off to shower. During this time, clean or inspect any incisions you may have on your legs.
- TED stockings are generally worn until you are back to your baseline activity. It may be longer or shorter depending on medications you are on to prevent blood clots; examination of your legs; medical history and your risk of blood clots. Discuss this question during your first follow-up visit (one week after surgery).
Should I have an extra pair of stockings and if so, where do I get them?
You will go home with one pair. You can purchase additional pairs in a medical supply store or some drug stores.
Is sizing of the stockings important?
TED stockings are ordered in small, medium and large and are sized based on the measurement of around the calf (circumference) and the length of the legs. The stocking should feel snug. These are different from prescription compression stockings which require a prescription for amount of pressure and sizing is measured by a clinician.
DVT Prevention
Deep Vein Thrombosis (DVT) is a blood clot that develops in a vein deep in the body. The clot may partially or completely block blood flow through the vein. Most DVTs occur in the lower leg, thigh or pelvis, although they also can occur in other parts of the body including the arm, brain, intestines, liver or kidney. DVT itself is not life-threatening. But, the danger of DVT is that the blood clot has the potential to break free and travel through the bloodstream, where it can become lodged in the blood vessels of the lung. This is a condition known as a pulmonary embolism. This can be life threatening, so prompt diagnosis and treatment is critical.
You are at risk for DVT if you:
- Have had recent surgery (generally within 3 months)
- Have been on prolonged bed rest or hospitalization
- Have heart failure
- Have a blood clotting disorder
While you were in the hospital your medical team checked you for DVT (physical examination and in some patients, an ultrasound) and would have started DVT prevention efforts. These might have included injections of a blood thinner under your skin, stockings that pump up and down on your legs known as intermittent pneumatic compression devices or white thigh high or knee high stockings. When you leave the hospital, you will need to prevent DVT from occurring until you are no longer at risk.
What to do when you leave the hospital:
1. Look out for symptoms of DVT.
Not everyone has symptoms of DVT, however be on the look out for:
- Swelling of the leg or arm (sometimes it occurs suddenly)
- Pain or tenderness in the leg that may only be present when standing or walking
- Feeling of increased warmth in the area of the leg or arm that is swollen or that hurts
- Redness or discoloration of the skin
- Enlargement of the superficial veins in the affected leg or arm
If you have symptoms of DVT, notify your doctor immediately or go to the emergency room. Do not wait to see if the symptoms “go away.”
2. You may be placed on medications (at home) to prevent or treat blood clots.
These should be taken as directed by your doctor. Keep your follow up appointments for lab work and your doctor so that your response to medications can be evaluated.
3. Wear your compression stockings as recommended by your doctor (see compression stockings tab).
4. Increase your activity.
- Exercise your lower leg muscles. If you are able, get out of bed, sit in a chair and walk every hour for at least a few minutes. The sooner you move around after you leave the hospital, the less chance you have to develop a clot.
- Don’t wear tight fitting clothing that could decrease the circulation in your legs.