What is Leukemia?
Leukemia is a type of cancer that develops in the bone marrow. Instead of causing tumors like other cancers, leukemia causes abnormal white blood cells to be overproduced. These are carried throughout the body.
In the bone marrow, stem cells produce different types of blood cells:
- White blood cells to fight infection
- Red blood cells to carry oxygen to tissues throughout the body
- Platelets to help the body to form a clot
In leukemia, white blood cells do not mature normally and are unable to fight infection. As the abnormal white cells accumulate, they interfere with the production of other blood cells. Eventually, the body produces too few red cells, too few platelets and too few healthy white cells. As a result, people with leukemia are at risk for infections, bruising and bleeding. Unless leukemia is diagnosed and treated properly, it can be fatal.
Is there more than one kind of leukemia?
Leukemia has many types and subtypes, classified by the type of white blood cell involved. The two main
types are:
- Lymphoid, or lymphocytic, leukemias (affecting bone marrow cells destined to become infection-fighting lymphocytes)
- Myeloid, or myelogenous, leukemias (affecting bone marrow cells destined to become red blood cells, plus other white blood cells and platelets) Depending on whether it is lymphoid or myeloid, leukemia can progress at different rates:
- Acute leukemia makes you sick very quickly, mainly by preventing healthy but immature white cells from maturing, rapidly reducing the body’s immune defenses.
- Chronic leukemia progresses more slowly, so the body retains some healthy cells to fight infection for a while.
Childhood Leukemia – Common Subtypes
- Acute Lymphocytic Leukemia (ALL) — 80% of children with leukemia have ALL, the most common childhood cancer.
- Acute myeloid, or myelogenous, leukemia (AML) — Fewer than 10-15% of children with leukemia have AML.
- Chronic myeloid, or myelogenous, leukemia (CML) — About 2% to 4% of CML occurs in children; CML most often affects adults.
- Juvenile myelomonocytic leukemia (JMML or JCML) — This rare form of leukemia generally affects children ages 2 to 5, but some of patients are diagnosed shortly after birth
Leukemia Symptoms
Symptoms vary, based on the leukemia subtype involved, and may include:
- Easy bruising or bleeding — Bleeding from the gums or nose or blood in the stool or urine, and bruising from very minor bumps
- Weakness or fatigue — Tiring easily because of lack of red blood cells
- Pallor — An unhealthy, pale appearance
- Susceptibility to infections — Increased risk of sore throats, pneumonia and other infections, sometimes with headache, low—grade fever, mouth sores or skin rash
- Swollen lymph nodes — Enlargement of the small, bean—sized nodes in the throat, armpits or groin that contain clusters of lymphocytes
- Loss of appetite and weight
- Discomfort in the belly — Pain below the left lower rib cage is most common
- Fever and night sweats
- Bone or joint pain
Leukemia Diagnosis

A pediatrician may find signs of leukemia during a physical examination. If your child has pallor, enlarged lymph nodes, swollen gums, an enlarged liver or spleen, significant bruising, pallor, or a small pinpoint rash, the doctor will order a blood test.
When blood tests show an abnormal white cell count, your child will be referred to a pediatric hematologist/oncologist, who specializes in childhood cancers. The oncologist will take a small sample of bone marrow tissue (a biopsy) to confirm the diagnosis and identify the leukemia subtype.
When bone marrow biopsies or other procedures are needed to diagnose cancer or monitor the effectiveness of treatment, Cleveland Clinic Children’s and other advanced centers rely on pediatric anesthesiologists. They put children to sleep so that they do not experience any discomfort.
Leukemia Treatments
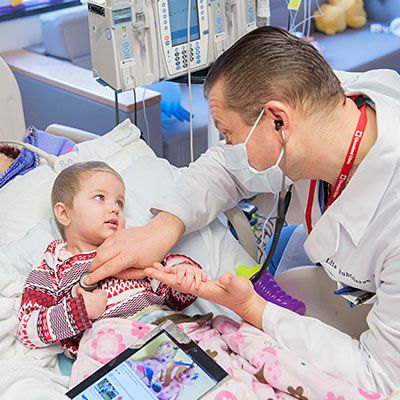
Treating leukemia requires immediate treatment with chemotherapy. Sometimes radiation therapy and/or blood and hematopoietic stem cell transplantation (HSCT) are also needed. The appropriate treatment depends on the subtype and certain distinct features of leukemia involved.
Chemotherapy.
Because leukemia is a systemic disease affecting the whole body,
chemotherapy is the best way to reach malignant cells throughout the body. Most
children are hospitalized upon diagnosis so that chemotherapy can begin safely and
without delay.
In the hospital, some chemotherapy drugs are given by catheter so that they are distributed through the bloodstream to the entire body. Other chemotherapy drugs are given in pill or liquid form.
Drugs may also be injected into the cerebrospinal fluid (CSF) surrounding the brain and spine to treat cancer cells or for prevention. This procedure is done by an oncology physician or a certified nurse practitioner while the patient is asleep so that there is no discomfort. Chemotherapy may be given in outpatient settings through an IV catheter, or in pill or liquid form.
Radiation therapy.
Radiation can be used to target specific areas where leukemia
cells can harbor, such as the brain or the spinal canal, since chemotherapy may
not penetrate the blood-brain barrier well. The entire body may be radiated prior to
HSCT.
HSCT.
In leukemia, high doses of chemotherapy or radiation may be used to eradicate
the bone marrow that is producing abnormal white blood cells. Healthy donor
hematopoietic stem cells are then introduced by IV catheter to create a new bone
marrow that eventually develops new white cells, red blood cells and platelets, as
well as a new immune system.
Leukemia Sub-types – Typical & Advanced Treatments
Acute lymphocytic leukemia (ALL)
- Typical Treatment — Several weeks of chemotherapy in the hospital followed by outpatient chemotherapy for months and low-dose maintenance therapy for years. Some children may require radiation therapy for about one month.
- Advanced Treatment — More than 90% of children treated for ALL achieve remission. The small percentage of patients whose ALL recurs can be retreated by chemotherapy alone or HSCT, depending upon timing and location.
Acute myeloid leukemia (AML)
- Typical Treatment — Several cycles, each a few weeks long, of chemotherapy in the hospital.
- Advanced Treatment — For certain types of AML with high-risk features or that do not respond well to chemotherapy, HSCT offers the best chance of remission or cure.
Chronic myeloid, or myelogenous, leukemia (CML)
- Typical Treatment — First-line therapy is lifelong treatment with a class of medications called tyrosine-kinase inhibitors.
- Advanced Treatment — Patients who cannot tolerate or do not respond to tyrosine-kinase inhibitors may be treated with HSCT.
Juvenile myelomonocytic leukemia (JMML)
- Typical Treatment — BMT is the most effective treatment, producing remission in about half of all children. However, the rate of relapse is high.
- Advanced Treatment — For children relapse, advanced centers offer access to clinical trials of new or different treatment approaches. The pediatric oncologist discusses all potential treatments and research studies with parents.
What is Lymphoma?
Lymphoma is the third most common cancer in children, adolescents and young adults. It develops in lymphoid tissue, found in the lymph nodes, tonsils, spleen and thymus gland. Because the lymphoid tissue is found throughout the body, lymphoma can start anywhere and spread to any organ, including the liver, bone marrow, spleen, lungs and skin.
When does lymphoma usually develop?
The two main types of lymphoma, Hodgkin’s lymphoma (once called Hodgkin’s disease) and non-Hodgkin’s lymphoma, develop at different ages:
Hodgkin’s lymphoma primarily affects teens and young adults (ages 13 to 39) and rarely occurs in younger children.
Non-Hodgkin’s lymphoma can occur at any age but usually develops between ages 7 and 11. It is two to three times more common in boys than in girls and affects more Caucasians than other races.
The four major subtypes of non-Hodgkin’s lymphoma most frequently affecting children and adolescents are shown below. Frequency may vary in different age groups.
B-cell non-Hodgkin’s lymphoma (Burkitt and Burkitt-like lymphoma)
- Incidence — About 40% of childhood lymphomas.
- Characteristics — Lymph node swelling in the neck, or inside the chest and abdomen; may involve the bone marrow and central nervous system.
Lymphoblastic Lymphoma
- Incidence — About 30% of childhood lymphomas
- Characteristics — A mass inside the mediastinum due to lymph node swelling in the chest and lymph node swelling in the neck; may involve the bone marrow and central nervous system
Anaplastic Large-Cell Lymphoma
- Incidence — About 20% of childhood lymphomas
- Characteristics — Lymph node swelling in the neck, or inside the chest and abdomen; may involve the bone marrow, central nervous system and skin
Diffuse Large B-Cell Lymphoma
- Incidence — About 10% of childhood lymphomas
- Characteristics — Most frequently involves the chest and abdomen, and may occasionally involve the bone marrow and central nervous system.
Lymphoma Symptoms
Both Hodgkin’s lymphoma and non-Hodgkin’s lymphoma may cause fatigue, loss of appetite, pain and weight loss. But other symptoms vary:
- Hodgkin’s lymphoma tends to produce swelling in lymph nodes within the neck, armpit or in the abdomen, and may also cause fever, night sweats and weight loss.
- Non-Hodgkin’s lymphoma develops in lymph cells deep within the body.
Swelling and other symptoms depend upon the primary tumor’s location:
- Spleen: May cause abdominal pain and organ enlargement.
- Thymus gland: May cause swelling of the face, neck or upper body. Cough and shortness of breath may also develop, which worsen when lying down or during physical activity.
- Near the superior vena cava: Because this major vein runs inside the chest to return blood from the head and upper extremities, lymphoma masses near the vein may cause headache, dizziness and loss of consciousness — a medical emergency
Lymphoma Diagnosis

Lymphoma is often discovered by your child’s pediatrician or family doctor. Lymph nodes in children and adolescents often swell in response to infection. When enlarged lymph nodes and unusual areas of swelling are found during routine examination, a course of antibiotics may first be prescribed.
If a child’s nodes persist or continue to grow, the doctor may order one or more types of imaging tests:
- A chest X-ray to get a closer look at structures inside the chest.
- A CT (computed tomography) scan, a sophisticated type of X-ray, to look at lymph nodes in the neck, chest, abdomen or pelvis.
- An MRI (magnetic resonance imaging) scan to determine whether the brain or spinal cord are involved.
None of these tests are painful, but children may require light anesthesia to help them hold still.
If imaging tests results are concerning for lymphoma, then your child will be referred to a pediatric oncologist. To distinguish an infection from lymphoma or other conditions, the doctor may recommend lymph node biopsy to examine the tissue under a microscope.
Biopsies can be done by withdrawing tissue from a swollen lymph node with a fine needle or by surgically removing the lymph node. At advanced centers like Cleveland Clinic Children’s, pediatric anesthesiologists make sure that biopsies are painless.
Hodgkin's & Non-Hodgkin's Management
Hodgkin’s and non-Hodgkin’s lymphomas are managed differently. In both
types of lymphoma, certain criteria can affect treatment:
- Tumor size
- Number of sites in the body affected by lymphoma
- Symptoms at diagnosis (such as presence of weight loss, night sweats or recurrent fevers)
- The patient’s age
- Pre-existing conditions increasing risk of long-term side effects
- Certain genetic features of the lymphoma cells
- Whether the lymphoma is newly diagnosed, unresponsive to prior treatment or recurrent following completion of the treatment
Hodgkin's & Non-Hodgkin's Treatments
Chemotherapy
Chemotherapy is generally used to treat Hodgkin’s lymphomas.
At Cleveland Clinic Children’s and other advanced centers, pediatric
oncologists are researching methods for safely shortening the duration of
chemotherapy if young patients have responded well early on.
Radiation therapy
For some patients, radiation is combined with
chemotherapy to eliminate any remaining cancer cells and reduce the risk
of recurrence. Radiation is also used to reach sites that respond poorly to
chemotherapy alone, such as the lungs, spleen and mediastinum.
HSCT
Hodgkin’s lymphoma has a high rate of cure. But if your child
should experience a relapse of the disease, his or her own hematopoietic
stem cells (also known as autologous stem cells) collected between cycles
of chemotherapy, can be transplanted to consolidate the treatment effect.
This approach can be highly effective in treatment-resistant situations as
well.
Many clinical trials are available for different stages of Hodgkin’s lymphoma. When pediatric oncologists at Cleveland Clinic Children’s and other advanced centers think young patients may benefit from participating in a such a trial, they will discuss all options with the family in detail.
Non-Hodgkin’s lymphoma may simultaneously involve multiple organs in the body, so your child’s oncologist will first stage the tumor to determine the best treatment. This is normally done through biopsy or imaging with CT (computed tomography), MRI (magnetic resonance imaging) or PET (positron emission tomography). Your doctor will tailor your child’s treatment depending upon the cancer stage and other factors.
Chemotherapy
Treatment for non-Hodgkin’s lymphoma involves giving
several chemotherapy drugs over a period of time to shrink tumors,
especially those that are large. The drugs are usually given on an outpatient
basis in cycles of several weeks, punctuated by periods of rest.
The outlook for non-Hodgkin’s lymphoma depends upon many things, including the lymphoma subtype, stage at diagnosis as well as certain laboratory parameters. Your pediatric oncologist will discuss your child’s progress with you throughout treatment and recommend the best options for an optimal outcome.
HSCT and CAR-T cell immune therapy
Depending upon the type of
lymphoma as well as initial response to standard first-line therapy,
some patients may further benefit from hematopoietic stem cell transplantation.
The stem cells will be harvested from a donor (allogeneic
stem cells) and not from the patient himself (like for Hodgkin’s lymphoma).
At Cleveland Clinic, some patients may also receive a very
innovative immune therapy with chimeric antigen receptor (CAR)-
modified T cells to precisely target the lymphoma cells.
Hematopoietic Stem Cell Transplantation

Cleveland Clinic has offered hematopoietic stem cell transplant, a complex but lifesaving treatment, since 1977. Today, Cleveland Clinic Children’s Blood and Marrow Transplant Program offers hope for children and adolescents with:
- Malignant diseases such as leukemia and lymphoma
- Non-malignant disorders such as severe combined immunodeficiency disease
- Hematological diseases such as sickle cell disease and thalassemia
New alternatives when they’re most needed.
When HSCT offers the only chance of cure, Cleveland Clinic Children’s collaborates with other centers across the nation to prepare patients using the most effective technique with the fewest side effects.
Our oncologists participate in clinical trials offered by the Blood and Marrow Transplant Clinical Trials Network (BMT CTN) and develop novel therapies with other centers participating in the Non-Myeloablative Transplant Consortium.
Reduced-intensity hematopoietic stem cell transplant is one example of a novel therapy available for certain categories of patients who:
- Have organ damage and are too sick to tolerate traditional HSCT
- Relapse after one HSCT and cannot tolerate another full-intensity transplant
- Have severe combined immunodeficiency disease
Another novel approach is to use the stem cells from either of the parents (also known as haplo-identical HSCT). It allows for no waiting for the donor to be identified, as well as enables the HSCT team to collect the stem cells more than once, if needed.
Finding the best match.
Our specialists help children and adolescents find the best possible marrow donor match through precise tissue-typing in Cleveland Clinic Taussig Cancer Institute’s sophisticated laboratory. When an appropriately matched adult donor (related or unrelated) cannot be found, Cleveland Clinic Children’s specialists use stem cells from stored umbilical cord blood to create less-than-perfect matches.
Meanwhile, our HSCT specialists continue to research genetic markers to find better ways of identifying excellent matches from unrelated donors.
Research
We no longer face grim survival rates for childhood cancers such as leukemia. ALL, Hodgkin’s lymphoma and other childhood cancers are now highly treatable, thanks in large part to clinical trials.
Clinical trials are not experiments. Clinical trials offer a means of comparing known treatments with other treatments that appear to have an even greater potential for success, while having a measurably lower side effect potential. The result can save lives or improve the quality of life.
Cleveland Clinic Children’s offers a number of pediatric cancer treatment protocols through the Children’s Oncology Group (COG), an international collaborative group dedicated to curing and preventing childhood and adolescent cancers. Your pediatric oncologist will explain whether your child may benefit from taking part in a clinical trial when he or she discusses your treatment plan with you.
Patient Services
MyChart.Caregiver
Parents and caregivers of children under age 18 can view test results, renew prescriptions,
review past appointments and request new ones using Cleveland Clinic MyChart.Caregiver®.
This secure online healthcare management tool connects parents and legal guardians to portions
of a child’s medical record at any time, day or night.
Medical Concierge
For complimentary assistance for out-of-state patients and families, call 800.223.2273, ext.
55580, or email
Global Patient Services
For complimentary assistance for international patients and families, please call the International
Patient Access Office at 216.444.8184. If you are calling from inside the United States, call
toll free at 866.320.4573.
Appointments and Locations
Make an appointment
For a same-day appointment with a Cleveland Clinic Children’s oncologist, please call 216.444.5517 or visit clevelandclinicchildrens.org/hemonc.
Visit us online
- Discover the many conditions our pediatric hematologists and oncologists treat and meet the talented experts on our team
- Learn more about our children’s hospital
Locations
Virtual Second Opinion
If you cannot travel to Cleveland Clinic, help is available. You can connect with Cleveland Clinic specialists from any location in the world via a phone, tablet, or computer, eliminating the burden of travel time and other obstacles. If you’re facing a significant medical condition or treatment such as surgery, this program provides virtual access to a Cleveland Clinic physician who will review the diagnosis and treatment plan. Following a comprehensive evaluation of medical records and labs, you’ll receive an educational second opinion from an expert in their medical condition covering diagnosis, treatment options or alternatives as well as recommendations regarding future therapeutic considerations. You’ll also have the unique opportunity to speak with the physician expert directly to address questions or concerns.
Why Choose Us?
Offering hope for your child and family
It’s difficult to hear that a child or teen has been diagnosed with leukemia or lymphoma. Yet there is cause for hope. Today, nearly 80 percent of the children and adolescents who are diagnosed with cancer can be cured. And for two of the most common childhood cancers, acute lymphocytic leukemia (ALL) and Hodgkin’s lymphoma, the success rates are even higher.
Young leukemia and lymphoma patients will find themselves in expert hands at Cleveland Clinic Children’s. Our team of pediatric hematologists/oncologists, radiation oncologists, surgeons, radiologists, specialized cancer nurses, social workers and nutritionists provides leading-edge yet family-friendly care. To achieve the best possible outcomes, we offer the most advanced diagnostic techniques and treatments, as well as access to the latest clinical trials and research protocols.
Our young patients have access to the extraordinary resources of Cleveland Clinic’s Taussig Cancer Institute. Cleveland Clinic children’s oncologists offer follow-up care into adulthood, and if desired, can then smoothly transition a child’s care to an adult oncologist.
Cleveland Clinic Children’s: Family-friendly care
Because cancer affects the entire family, providing great medical care is just part of our mission at Cleveland Clinic Children’s. We have social workers, pediatric psychologists, child life specialists, art therapists and other caregivers on our team to help families cope. We also offer the following special services:
Sibling Outreach Program: This addresses the psychosocial and educational needs of a young patient’s brothers and sisters, and allows siblings from different families to meet one another and enjoy activities together.
‘High Five’ Cancer Survivors’ Clinic: This provides long-term follow-up care for young cancer patients. Its staff coordinates multidisciplinary treatment as a child grows up, providing vital information for cancer survivors going off to college or entering adulthood.
Children’s Cancer Answer Line: This service allows anyone in your family to talk with a pediatric oncologist or nurse. Call 216.444.5517 or 800.223.2273, ext. 45517, between 8 a.m. and 5 p.m. weekdays. (Select option 1.)

