A lumbar puncture (spinal tap) is a diagnostic procedure where a healthcare provider removes cerebrospinal fluid from your spine. You won’t feel the procedure as it happens, as you’ll receive an anesthetic. A spinal tap can diagnose conditions that affect your brain, nerves and spinal cord like meningitis, leukemia and encephalitis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
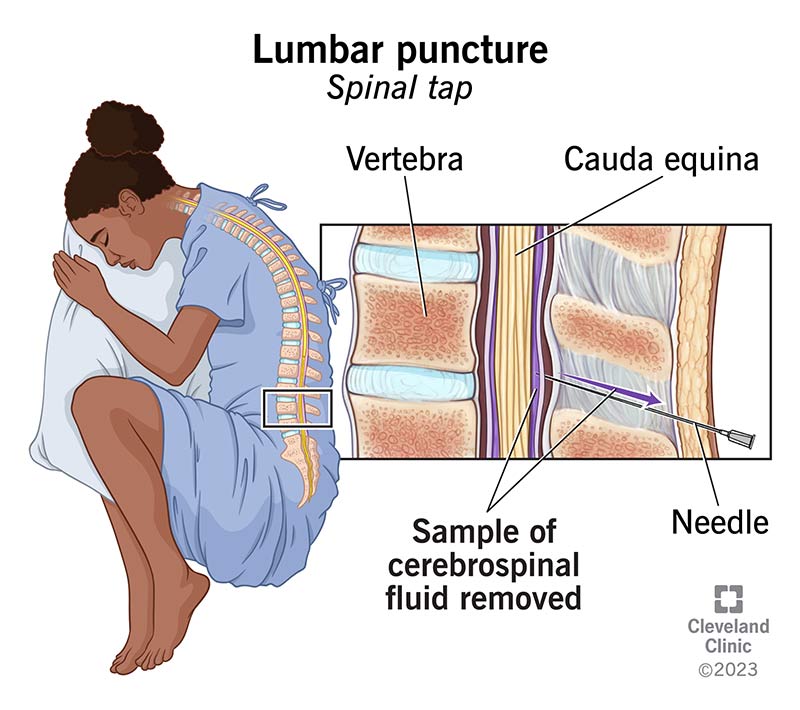
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/12544-lumbar-puncture-spinal-tap)
A lumbar puncture (spinal tap) is a procedure where a healthcare provider inserts a needle into your lower back to remove a sample of cerebrospinal fluid. Cerebrospinal fluid is the clear fluid that surrounds your spine and brain.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This test can help diagnose conditions that affect your brain, nerves and spinal cord.
Your healthcare provider may perform a lumbar puncture to test for:
Healthcare providers also use a lumbar puncture (spinal tap) to:
This isn’t an exhaustive list of all conditions and reasons for the procedure. Your healthcare provider can give you the best information as to why they need to perform this procedure.
If your healthcare provider schedules a lumbar puncture, they may recommend the following before your test, in addition to a physical exam and learning more about your health history:
Advertisement
These preparations help your healthcare provider learn more about the area of your body that they’ll be looking at during the procedure, make sure it’s safe for you and take steps to prevent complications.
Your provider will give you specific or additional instructions to help you prepare.
For a lumbar puncture, a healthcare provider will instruct you to lie on your side (usually the left side). You’ll need to pull your knees to your chest when they’re ready and stay in that position for the length of the test. Or you may sit and lean forward with your arms and head resting on a table. While this position may be awkward or uncomfortable, it’s important that you stay as still as you can and follow their instructions. You may need to change your position slightly during the procedure.
Next, your provider will clean your skin and numb the area of your lower back with a local anesthetic. You might feel a slight burning sensation when you get the anesthesia. You won’t feel any pain during the procedure, but you may feel pressure.
When the area of your body is numb, your provider will insert a thin, hollow needle in between two vertebrae (usually the third and fourth lumbar vertebrae). This is in your lower back above your buttocks. The needle will move into the subarachnoid space or the area between your spinal cord and the meninges (membrane layers that cover your spinal cord). Your provider may use an X-ray called a fluoroscopy to help guide the needle to the correct spot.
Once the needle is in place, your healthcare provider will measure spinal fluid pressure and remove a sample of cerebrospinal fluid.
When your provider completes the procedure, they’ll remove the needle and put a bandage on your skin.
Depending on your situation, a spinal tap may take place as an outpatient procedure (you go home the same day) in a medical office or in the hospital. If you have an outpatient procedure, someone needs to drive you home afterward.
No. You’ll receive local anesthesia, not general anesthesia, so you’ll be awake during the procedure. But you won’t feel any pain.
A lumbar puncture takes about 15 to 30 minutes from start to finish. The needle is only in your back for a few minutes.
After a lumbar puncture, your healthcare provider will give you instructions to take care of yourself. This may include the following after the procedure:
With your provider’s OK, you may be able to return to work after a spinal tap.
About 10% of people who get a lumbar puncture develop a spinal headache. This feels like intense pain when sitting or standing. A headache may come on within hours or several days after the procedure. The pain typically goes away on its own in a couple of days, but it may linger for a week or more. Along with the spinal headache, you may experience:
Advertisement
Over-the-counter pain medicines, staying hydrated and drinking caffeinated beverages can help.
Side effects after a lumbar puncture are rare and may include:
There’s no risk of spinal cord damage after a lumbar puncture. Your cord sits higher than the area of the lumbar spine area where the spinal tap takes place.
A lab tests the cerebrospinal fluid sample after a lumbar puncture to check for:
These results help your healthcare provider rule out and diagnose possible conditions.
The timing of spinal tap results depends on the reason for the test. On average, you should get your results within two to three days. If you need an emergency spinal tap to check for life-threatening conditions like a brain bleed or meningitis, you’ll get your results sooner.
As a spinal tap helps diagnose multiple possible conditions that affect your brain, nerves and spinal cord, results vary based on what they show. For example, if you have a high white blood cell count, you may have an infection. Antibiotics can treat the infection so you feel better.
Advertisement
Your healthcare provider will explain what your results mean and what the next steps are to treat any underlying conditions.
You should call your healthcare provider if you experience:
A procedure that involves sticking a needle into your spine may sound scary, but a lumbar puncture, or spinal tap, carries little risk. You won’t feel any pain during the procedure. But you may feel some pressure in your lower back. Talk to your healthcare provider about any concerns you have before, during or after your procedure. If you develop a spinal headache, your provider can offer suggestions to feel better.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.