If you have abdominal pain below your belly button, your healthcare provider might call it lower abdominal pain. Dividing the abdomen into regions helps narrow down the many causes of abdominal pain.
Abdominal pain has many causes and may involve many different organs. To help narrow it down, healthcare providers often think of the abdomen in regions. Your lower abdomen is the portion that falls under your belly button. Lower abdominal pain may involve any of the organs that live between your belly button and your pubic bone. This includes abdominal organs and pelvic organs. With pain, it can be hard to tell the difference.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Lower abdominal pain is most likely to come from one of the organs in your lower abdominopelvic cavity. These include your:
Less commonly, pain may be referred from somewhere else in your body if it triggers nerves that travel between the two areas. Your kidneys live in the back of your abdominopelvic cavity, but pain in your kidneys may wrap around to the front. People with testicles may feel testicular pain in their abdomen.
Abdominal pain can be acute or chronic, and so can its causes. Acute causes occur suddenly, and they’re usually temporary. They include injuries and most infections. Chronic diseases can cause chronic pain that persists for a long time or that comes and goes. Both types of pain can become progressively worse. This can be a sign that the disease is also getting worse. Seek urgent care for severe or progressive pain.
Some causes are serious and some aren’t. It can be hard to tell from the way you feel. If your pain is severe or getting worse, it’s worth seeking medical care regardless of what’s causing it. A healthcare provider can help relieve your pain while also investigating the cause. If you’ve had chronic pain for a while and you don’t know why, that’s also worth investigating, even if it doesn’t feel too severe.
Most of your small and large intestines are in your lower abdominal cavity, and they take up most of the space in there. For this reason, conditions affecting your intestines are the most common causes of lower abdominal pain. These include everyday digestive problems such as gas and indigestion, diarrhea and constipation. They also include more serious gastrointestinal diseases, both chronic and acute.
You may have indigestion, gas or problems with your poop if you have a food allergy or intolerance, or if your digestive system isn’t working right. Many things can interfere with the digestive process. You may also feel pain if your intestines are inflamed, which happens when your immune system is activated. Inflammation in your small intestine (enteritis) or in your large intestine (colitis) may be caused by:
If you have female reproductive organs, these also live in your lower abdominopelvic region. These organs are another common cause of lower abdominal pain. After all, it can be hard to tell the difference between intestinal cramps and menstrual cramps because your uterus and intestines are so close together. While some period pain is normal, it can sometimes indicate a problem, such as:
You also may feel pain in your ovaries if you have:
When your digestive system or your female reproductive system isn’t involved, you may have pain originating from your urinary system. A urinary tract infection is a common cause of pain in your bladder or ureters. Kidney infections may cause lower abdominal pain if it radiates from your back. You may also have bladder inflammation or kidney pain from other irritations or diseases.
Lower left abdominal pain is often related to diverticulosis and diverticulitis of the colon. Diverticula, pouches that develop in your colon wall, most often occur on the lower left side. These pouches make great hiding places for bacteria and can easily become infected, causing inflammation and pain.
Lower right abdominal pain may be related to your appendix, which branches off to the right from your large intestine. Inflammation in your appendix (appendicitis) is a common cause of lower abdominal pain. An inflamed appendix can also burst, spreading infection to your peritoneum (peritonitis).
You may also have lower abdominal pain on one side if you have a condition affecting one ovary or one kidney. A growth, such as a tumor or a cyst, may occur in one ovary or one kidney on either side. A kidney stone usually affects one kidney at a time. Ovulation pain usually affects one ovary at a time.
You can treat milder pain at home with over-the-counter (OTC) analgesics, such as NSAIDs and acetaminophen. Or you may need prescription pain relievers, such as steroids or opioids, depending on your condition. If you go to the hospital with severe pain, they might give you medication through an IV. They’ll also look to isolate and treat the underlying cause of your pain, which might be many things.
The most common causes of lower abdominal pain aren’t serious. You can often treat intestinal or menstrual cramps at home with rest, heat and hydration. Try giving your digestive system a rest if it’s bothering you, and stick to broths and teas for a day. Herbal teas such as peppermint, licorice, and ginger can help soothe your digestive system. In the longer term, you might want to adjust your diet.
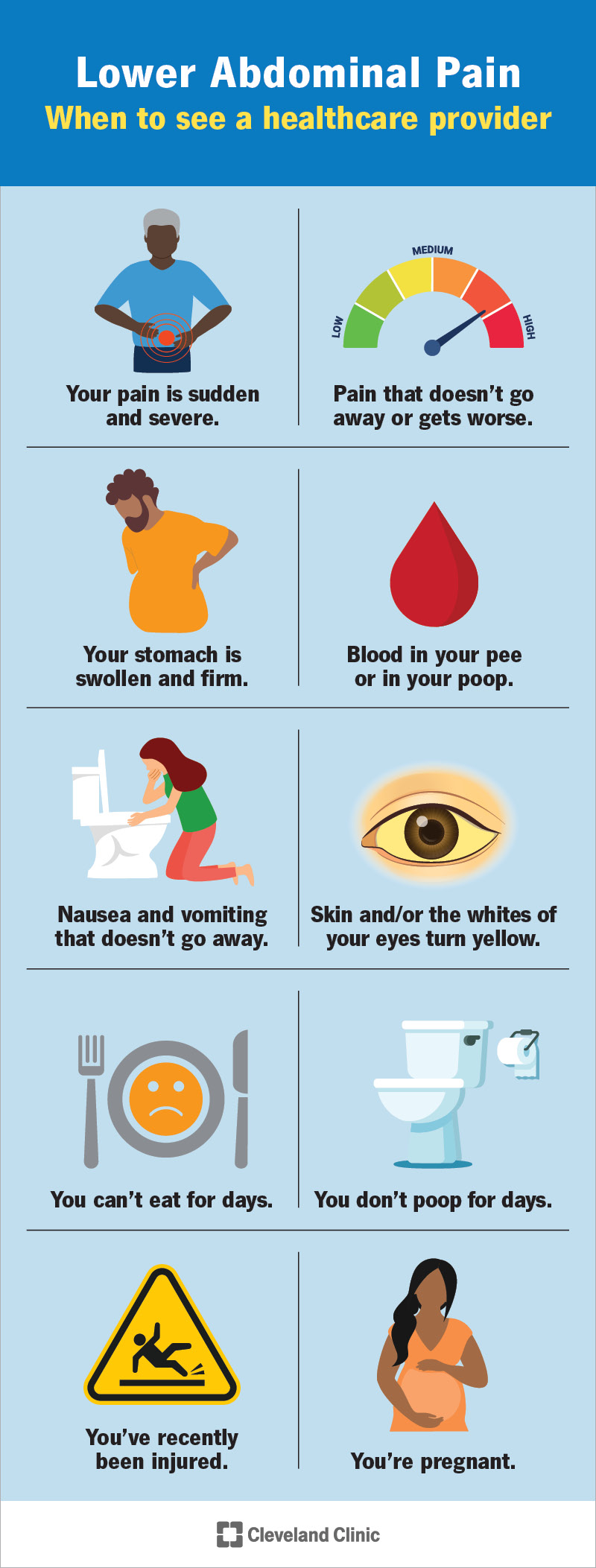
See a healthcare provider if:
A note from Cleveland Clinic
Lower abdominal pain is common, but sometimes it’s hard to tell what’s hurting. You may have a hunch if your symptoms follow your digestive cycle or your menstrual cycle. You may be able to identify an infection in one of your organs by the other symptoms it brings along with pain. Less common and less recognizable diseases and conditions may need a healthcare provider to diagnose and treat them.
Last reviewed by a Cleveland Clinic medical professional on 12/12/2022.
Learn more about our editorial process.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy