Caring for eyes at an early age

You want to get your young children off to a good start in every way — and that includes their eye health. But when is the right time to start having your child’s eyes checked? Babies and toddlers can’t read an eye chart, after all. It’s best to start early.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It’s important not to delay eye exams for young infants and children because some early eye problems can affect vision for life. Finding a problem early can keep a minor issue from becoming something major (and harder to treat).
Pediatric ophthalmologist Elias Traboulsi, MD, MEd, emphasizes that eye exams aren’t merely a way to know whether your child needs glasses. Like regular exams with a pediatrician, eye exams are about preventive care.
Dr. Traboulsi recommends a comprehensive eye exam by an eye care professional if possible by age 1, to be repeated before kindergarten in children without any evident eye problems. Pediatricians do perform limited eye examinations right after birth and in the first few years of life. These can detect a variety of abnormalities in the light reflex from the pupil and in the external aspects of the eye and the ocular alignment.
These exams become much more important in children who:
“Even if there are no obvious symptoms, your child may still have a problem with his vision,” he says.
Undiagnosed conditions or abnormalities can lead to vision loss. But it’s possible to reverse some problems if they’re caught early, Dr. Traboulsi says.
A classic example is lazy eye. Kids with this condition have one eye that is weaker than the other.
One of the most common vision problems in children, lazy eye typically responds well to treatment. This may include an eye patch, eye drops or eyeglasses.
Another example is crossed eyes, which involves one or both eyes turning inward or outward. This can require special eyewear or an eye patch.
So how do you know there’s a problem or your child needs to see a doctor?
Here are four key tips that will help you make sure your child has the best eye care from the start.
If you have questions about your young child’s vision, don’t hesitate to schedule an eye exam.
Most children have their vision tested before they start elementary school. But Dr. Traboulsi says it’s ideal to have your child’s eyes tested before they start kindergarten or preschool.
“While it’s ideal for all kids to have their eyes tested, it’s even more important if a child’s brothers or sisters have vision problems,” says Dr. Traboulsi.
As with many other health-related conditions, your child is more likely to have vision problems if they run in your family. So it’s best to start monitoring it early on.
As you know, your pediatrician has specialized training for treating children. By the same token, a pediatric ophthalmologist specializes in detecting and treating children’s eye problems.
With kid-friendly tools and testing, they can pinpoint problems — even if your child hasn’t learned how to talk or doesn’t yet know the alphabet.
Dr. Traboulsi says it’s very important for parents to trust their instincts. After all, you know your child best.
In fact, parents are often the first ones to notice signs of trouble. “If a mom says something is wrong with her child’s eyes or vision and I don’t find anything in the initial exam, I always go back and test again,” he says.
Your doctor may not find a problem at first. But if you still have concerns, keep working to pinpoint the problem. Discuss the signs you’re seeing with your child’s doctor or get a second opinion, if necessary, Dr. Traboulsi advises.
Following these tips will help you protect your child’s vision and promote healthy eyesight for life.
Learn more about our editorial process.
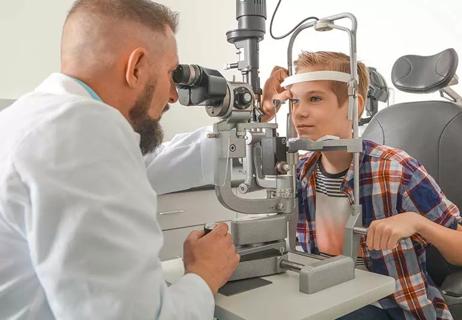
Plan on an annual vision screening, but a full exam may not be necessary

Your eyes can reveal many clues about underlying health issues

Preserving your social life and protecting your mental health are key to living well with vision loss

Start low-vision rehabilitation as soon as possible and see your retina specialist at least every six months

These trendy glasses might brighten some shades and help you see the difference between colors or brightness of hues, but they won’t cure your color vision deficiency
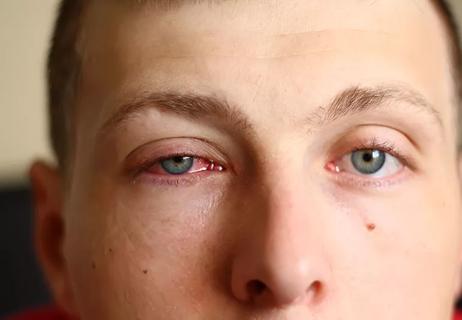
Eye drops and cold water rinses can help speed up healing for viral and allergen-related conjunctivitis, but a bacterial infection will need antibiotics

Your eye prescription reveals a lot about your eye health, including how they’re shaped, how well you see and what your new glasses can do for your sight

From scratching your cornea and tearing your retina to introducing allergens and causing infections, pawing at your peepers just doesn’t pay off

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses