A DEXA scan is an imaging test that measures bone density (strength). DEXA scan results can provide helpful details about your risk for osteoporosis (bone loss) and fractures (bone breaks). This test can also measure your body composition, such as body fat and muscle mass.
A bone density test, DEXA, measures the mineral content of the bones in certain areas of the skeleton. It’s a way to measure bone loss as you age. Healthcare providers sometimes call these tests bone densitometry tests, or DXA.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A DEXA scan is a type of medical imaging test. It uses very low levels of x-rays to measure how dense your bones are. DEXA stands for “dual-energy X-ray absorptiometry.”
Medical experts consider DEXA scans to be the most useful, easy, and inexpensive test for helping to diagnose osteoporosis. The test is quick and painless.
Osteoporosis is a term used to describe brittle bones and also the risk for having a broken bone. As you age, your bones can lose thickness and strength. Osteoporosis literally means “porous bone.” DEXA tests help your healthcare provider track your bone density and risk for having a broken bone over time. Providers often use DEXA tests to help diagnose osteoporosis.
Osteoporosis results when you to lose bone faster than your body can create new bone tissue. This is most common in postmenopausal women. Over time, bones get weaker. Brittle bones break more easily.
Providers sometimes call osteoporosis a “silent” disease because it doesn’t hurt. Many people first realize they have osteoporosis after they break a bone from a minor fall.
Osteopenia is a term used to describe “low bone mass.” Many individuals, including those who are slender and very active, have lower bone mass all of their lives. But this does not necessarily mean that they will develop osteoporosis. Many world-class athletes have low bone mass but their bones are healthy and very strong. Osteopenia is not “pre-osteoporosis,” but sometimes, if a person has other risk factors for fracture, an osteoporosis medication will be recommended to help prevent future fractures.
DEXA scans measure the mineral content in certain bones, such as the hip, spine and/or wrist. It works this way:
Healthcare providers consider many factors when deciding who may benefit from a DEXA scan and how often. Healthcare providers often recommend a DEXA scan to assess your bone health for osteoporosis and fracture risk if you are older than 50, have had a broken bone, or other illnesses that put your bone health at risk.
Research shows women start losing bone mass earlier and faster than men. So healthcare providers usually recommend women get a DEXA scan to screen for osteoporosis at younger ages compared to men.
Your provider may recommend a DEXA scan if you have one or more risk factors for osteoporosis or fractures:
Healthcare providers may also order a DEXA scan to:
Medicare allows a DEXA scan to be done once every two years, and this is the current recommended timeframe. There are exceptions to this rule if you have certain diseases.
Your healthcare provider will consider several factors, such as your age, level of fracture risk, previous DEXA scan and current medications. Your healthcare provider will then make a personalized plan for how to assess and protect your bone health.
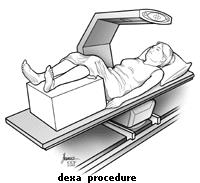
Most people don’t need to change their daily routine before a DEXA scan. Eat, drink and take any medications as you normally would, unless your provider tells you otherwise. You will be asked to fill out a questionnaire that asks about your current health, your family history of broken bones, smoking history, and current medications.
Before your test, please do the following:
DEXA bone density tests are outpatient procedures. You may be able to wear your regular clothes during the test. Or you may be asked to change into a hospital gown. There are no needles or injections in this test. Getting a DEXA test is similar to having a standard X-ray.
A DEXA scan usually takes no more than 25 minutes. Many people are in and out of the room in less than 30 minutes.
Not at all. You won’t feel a thing as the X-ray beams pass through your body.
You may feel slightly uncomfortable lying on the table, depending on how you’re positioned. But you’ll only need to stay in that position for a few minutes.
DEXA scans offer a high degree of precision and accuracy. Medical experts consider DEXA scans to be an accurate test for diagnosing osteoporosis.
Unlike x-ray machines, DEXA machines are checked daily for their ability to measure bone mineral accurately, and no two DXA machines are exactly alike. That is why your healthcare provider will insist that you have all of your DEXA tests done on the same machine.
DEXA scans are quick and painless. You should be able to resume your usual activities immediately after the test.
Professionals certified to interpret DEXA images will review your results and write a report that will be sent to your healthcare provider.
Your healthcare provider will explain your test results and help you understand what they mean for your health. Your healthcare provider can help you make decisions about how to keep your bones strong. They can also recommend diet and lifestyle changes that may help to lower your risk of a fracture.
If your healthcare provider has recommended a DEXA scan, you may want to ask:
Medical experts consider DEXA scans the “gold standard” for diagnosing osteoporosis and fracture risk. Many individuals lose bone density as they age. But that doesn’t mean you have to accept fragile bones simply as a reality of getting older. It is never too early to learn how to take care of your bones! Ask your provider if a DEXA scan may help assess your bone health today. Then, talk about steps you can take to slow bone loss or protect your bones for years to come.
Last reviewed by a Cleveland Clinic medical professional on 12/15/2020.
Learn more about our editorial process.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy