How to maintain your mobility well beyond retirement
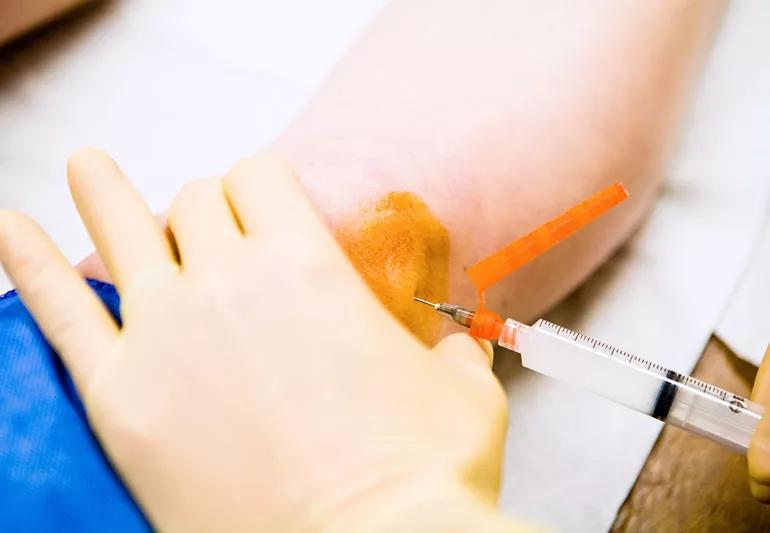
If you have recurring or chronic joint pain, you may think joint replacement surgery is your only option for relief. However, you may want to explore several less invasive options first to help maintain mobility as you age.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
With millions of people wanting to stay active into their 60s, 70s and beyond, much recent research has focused on joint health and replacement technology.
Experiencing joint pain doesn’t automatically mean that you should have a joint replacement, says orthopaedic surgeon Anthony Miniaci, MD.
“Joint replacement surgery is generally performed for late stages of degenerative arthritis (also called osteoarthritis), after other options have failed,” he says. Most causes for joint pain including knee, hip, shoulder and ankle can be treated with far less invasive options.
So how do you know your arthritis or other joint damage needs attention?
In general, you should see a doctor if your joint pain limits your activities for more than three days without improvement, or you have recurring episodes of the same pain over several weeks or months.
You can damage a joint suddenly. Or joint damage may come on gradually, bothering you periodically at first and becoming more painful over time.
The causes of joint pain may include:
Most causes for joint pain never require surgery. However, even in the case of osteoarthritis, surgery is not necessarily the first choice. Whatever the cause, you’ll want to preserve your joints for as long as you can.
This is particularly true if you are a younger, active person.
Joint replacement has gotten much safer and faster to recover from. You may leave the hospital on the same day or one day after surgery, but these are serious operations that are not to be undertaken lightly, says Dr Miniaci.
Joint replacement techniques and associated parts are thought to last longer than they used to. But they are mechanical and subject to loosening, stiffness, complications and infection. These problems may lead to follow-up surgeries down the road which are more complicated and generally not as successful as they are the first time.
“Most people now live into their 80s. Many of the next generation will live to be older and into their 90s,” Dr. Miniaci says. “If someone in their 50s is very active and has knee or hip joint replacement, they may need one or two more operations in their lifetime, so we try to avoid it until later if possible.”
The goal of preservation is to prevent injury, reduce inflammation and preserve cartilage, Dr. Miniaci says. These factors figure in when your physician weighs your options:
Some newer joint preservation procedures are considered experimental, Dr. Miniaci says. Physicians have used other preservation techniques for decades. Options include:
Injections of hyaluronic acid or corticosteroids can reduce inflammation in many patients in the lining of the joints. These treatments can work in most joints and have been well-studied and results are mixed. But not all insurance carriers will cover these injections.
Your blood contains platelets — hundreds of thousands of platelets are present in every milliliter of blood. These contain chemicals that can stimulate tissue repair, reduce inflammation and stimulate your own cells in the healing response.
Because of this, many clinicians have begun using injections of concentrated plasma which includes platelets from blood to treat inflamed or injured tendons, ligaments, muscle and joints.
In this technique, your treatment team will grow, transplant or use a cartilage replacement and place it in the damaged space. They can also stimulate the bone in your joint to increase cartilage growth. Not one technique is the proven best and much work needs to be done.
Physicians use this technique when there is damage to a smaller areas of your joint. The benefit to this technique is that the surgeon can preserve most of the bone with the use of smaller artificial parts to replace particular sections of your joint. This treatment works in many joints, but must be used carefully and does not work for all.
Replacement in one part of the joint does not necessarily prevent degeneration in other parts of the joint. As a result, partial replacements may not last as long as a full joint replacement but the benefit is still being able to do a full replacement in the future.
If you’ve unsuccessfully attempted conservative treatment or if damage to the cartilage or bone is beyond repair, remember that joint replacement is proven to be safe and highly effective in the right patient. Dr. Miniaci says this is still often your best option. Newer techniques in the hip and shoulder as well as knee can give patients excellent pain relief and improved function. However, there are always potential risks and complications with surgery.
Talk with your doctor about the best options and long-term strategies for you and understand what’s available for your specific problem. Preserving your joints and your activities and lifestyle is the basis for a partnership that is best for you.
Learn more about our editorial process.

They can last 10 to 15 years, but factors like age and activity level can impact their longevity
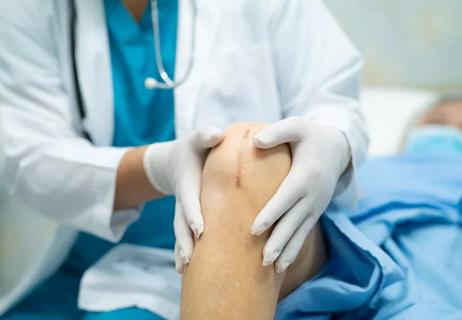
Hip and knee replacements are among the most successful and satisfying

Build a fitness program to keep your new hip or knee in good shape

Make a proactive plan to prepare yourself for surgery
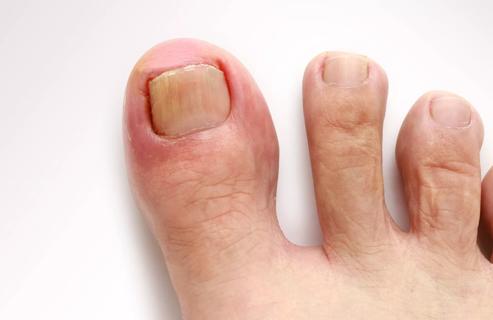
Pain meds, toenail protectors and petrolatum jelly may spare you a trip to a podiatrist

An ice bath can ease sore muscles and decrease inflammation after a workout

Wrist flexor and extensor stretches are the best stretches for wrist pain

Simple exercises like tendon glides and finger lifts can have a big impact

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses